Impact Factor ISSN: 1837-9664
J Cancer 2014; 5(6):465-471. doi:10.7150/jca.9235 This issue Cite
Research Paper
Activation of Angiogenesis Differs Strongly Between Pulmonary Carcinoids and Neuroendocrine Carinomas and Is Crucial for Carcinoid Tumourgenesis
1. Institute of Pathology, University Hospital Essen, University of Duisburg-Essen, Essen, Germany;
2. Ruhrlandklinik, West German Lung Center, University Hospital Essen, University of Duisburg-Essen, Essen, Germany;
3. Department of medical Oncology, University Hospital Essen, University of Duisburg-Essen, Essen, Germany;
4. Institute of Pathology, University Hospital Cologne, Cologne, Germany.
5. Pulmonary Department-Oncology Unit, ``G. Papanikolaou`` General Hospital, Aristotle University of Thessaloniki, Thessaloniki, Greece.
6. Department of Respiratory Diseases, Changhai Hospital/First Affiliated Hospital of the Second Military Medical University, Shanghai, People's Republic of China, China.
* Authors equally contributed.
Received 2014-3-27; Accepted 2014-4-1; Published 2014-5-15
Abstract
Background: Lung cancer still remains the leading cause of cancer for men after prostate cancer and breast cancer for women. Angiogenesis is considered a major microenvironment modifier. Material and Methods: Demographic data and study design; The study is based on a collective of twenty representative specimens of each tumour entity (Typical Carcinoid, Atypical Carcinoid, Large-Cell Neuroendocrine Carcinoma , Small Cell Lung Cancer) for mRNA expression analysis. The following methods were performed: RNA Extraction and RNA Integrity Assessment, NanoString CodeSet Design and Expression Quantification, NanoString Data Processing and Statistical Analysis. Results: KDR rendered significant association to aggressiveness of the tumour and decreases with increasing malignancy (p=0.049). A decreased expression of HIF1A and KDR mRNA as associated with a higher risk of tumour invasion in vessels (HIF1A: p=0.034; KDR: p=0.029). FIGF and HIF1A expression levels are significantly associated with progression-free survival (FIGF: p= 0.021; HIF1A: p= 0.049). CRHR2 and FLT4 are stronger expressed in female than in male patients (CRHR2: p=0.024, FLT4: p=0.004). FIGF expression is still significant between LCNEC and SCLC (p=0.023). FLT4 and KDR show highly significant association to one of the analysed groups (FLT4: p=0.001; KDR: p=0.006). Additionally, HIF1A expression differs significantly between these focus cohorts (p=0.018). Conclusion: We should consider for clinical practice application which factors affect most the tumour growth and distal metastasis, thereafter investigate easy to administer drugs with low side effects. Probably a cluster system of therapy should be established where a drug targets simultaneously different pathways of the same origin.
Keywords: lung cancer, HIF1A, FLT4, FIGF, carcinoid, KDR, CRHR2.
Introduction
Lung cancer is the leading cause of cancer-related deaths worldwide with a poor five-year survival prognosis of approximately 15% and accounts for more deaths than the next four lethal cancer types in sum [1-3]. Twenty-five percent of all lung tumours belong to the group of neuroendocrine tumours [4]. These pulmonary neuroendocrine tumours encompass the small-cell lung carcinoma (SCLC), large-cell neuroendocrine carcinoma (LCNEC), as well as the typical (TC) and atypical carcinoid (AC) [5]. Nevertheless the incidence of pulmonary carcinoids have increased over the past 30 years, their combined incidence in 2003 was just 1.57 per 100,000 inhabitants in the USA [6]. Patients suffering from typical carcinoids have excellent survival rates with 87-100%, but some present with lymph node metastasis (4-15%) [7-16]. Atypical carcinoids are more aggressive and show higher frequency of nodal metastasis (35-64%). The survival rate decreases to 61-88% [9-15, 17]. TC and AC patients mean age is 45-55 years [16].
LCNEC is an entity that was recognized for the first time only about one decade ago. On the one hand, LCNEC belongs to the non-SCLC tumours according to the WHO classification from 1999, but on the other hand it shows similar progression as SCLC with a five-year survival of 15% up to 57% depending on the reporting source [4, 9]. Up to 20% of all lung cancer incidences are SCLC cases, showing clear neuroendocrine features [4], and metastasize early [5, 9, 16]. Ninety-five percent of all small cell carcinomas (SCC) are found in the lung whereas non-pulmonary SCC are very rare [4]. The five-year survival for SCLC is <5% [4]. Even when diagnosed at an early stage, SCLC and LCNEC show the poorest clinical outcome compared to other lung tumours due to the aggressiveness of these cancer types, but still the molecular characteristics of these tumours remain largely unknown [5]. They grow very rapidly and occur almost exclusively in patients with a history of smoking, whereas lung carcinoids occur frequently in never smokers and younger patients [6, 8, 16, 18].
The diagnostic discrimination on morphological grounds of LCNEC versus atypical carcinomas and SCLCs is difficult due to overlapping features, so the diagnosis by immunohistochemical staining is a routine tool for differential diagnosis of neuroendocrine tumours. As with all subjective imaging methods these techniques are prone to significant intra- and interobserver variability reducing the reproducibility and reliability of this methodology [4, 9, 19, 20]. Furthermore, LCNEC and SCLC differentiation and TC and AC differentiation, respectively, by IHC is hindered by their related biological characteristics leading to false identification [4, 5, 9]. Only a 40% unanimous agreement among five pathologists diagnosing LCNEC was accomplished in a reproducibility study by Travis et al. [21]. Furthermore, in an interobserver variability study 12% unanimous diagnosis were made within nine pathologists [22].
Angiogenesis and lymphangiogenesis are important characteristics of aggressive tumours, resulting in metastasis [44, 45]. Yu et al. reported that increased expression of VEGFA and KDR (VEGFR-2) correlated with progression of the tumour [44]. Furthermore, they also identified HIF1A, a transcription factor that regulates genes that respond to hypoxia, to be overexpressed in lung cancer. They proposed that this might be due to the hypoxia environment of a tumour and that this might trigger angiogenesis [44]. FIGF is an activator of KDR and FLT4 (VEGFR-3) and induces angiogenesis and lymphangiogenesis [45].
Material and Methods
Demographic data and study design
The study is based on a collective of twenty representative specimens of each tumour entity (TC, AC, LCNEC, SCLC) for mRNA expression analysis. The initial diagnosis was re-evaluated by two experienced pathologists (JWO, THA). Inclusion criteria were sufficient tumour material and minimum of contamination by lymphocytic and stromal cells of the FFPE tissue. Specimens were collected at the Department of Pathology and Neuropathology at the University Hospital Essen, Germany from 2005 till 2012. TNM-staging was based on the WHO Classification Of Tumours guidelines (2004) [18]. The study was conducted retrospectively for the identification of biomarkers to distinguish different types of pulmonary neuroendocrine tumours. Patients that received chemotherapy before resection of tumour tissue specimens were excluded. The study was approved by the ethical committee of the University Hospital Essen (ID: 13-5382-BO). The investigation confirm to the principles outlined in the declaration of Helsinki.
RNA Extraction and RNA Integrity Assessment
Three to five paraffin sections with a thickness of 4 µm per sample were deparaffinised with xylene prior to RNA extraction using the RNeasy FFPE kit (Qiagen, Hilden, Germany) according to the manufacturer's recommendations. RNA concentration was measured using a Nanodrop 1000 instrument (Thermo Fisher Scientific, Waltham, USA). RNA integrity was assessed using an Agilent 2100 bioanalyzer (Agilent Technologies, Santa Clara, USA) at the NanoString nCounter Core Facility at the University of Heidelberg, Germany. Smear analysis was performed using the Agilent 2100 expert software to determine the proportion of RNA ≥300 nucleotides (nt) within a given sample.
NanoString CodeSet Design and Expression Quantification
Important genes for different tumour-associated signalling pathways and neuroendocrine differentiation were included in the CodeSet. The CodeSet was designed to contain a total of 91 genes with different signature genes for each subgroup. The investigated genes of the corresponding angiogenesis pathway contain CRHR2, FIGF, FLT4, HIF1A, KDR and MMP3. Three reference genes (ACTB, GAPDH, and HPRT1) were also included in the CodeSet for biological normalization purposes. An overview of all genes and their functions in an angiogenetic context is shown in Fig. 1.
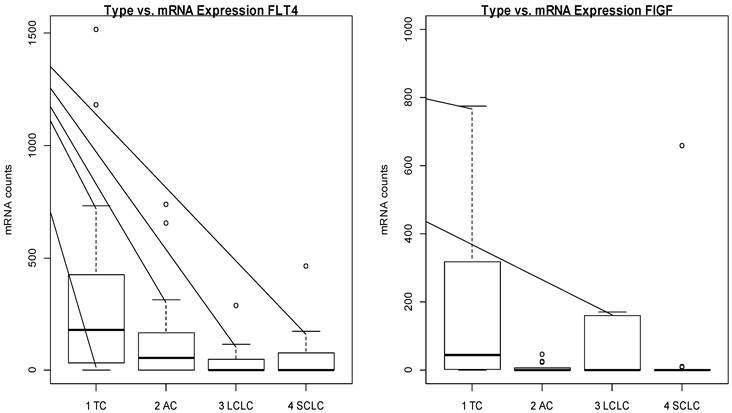
TC; typical carcinoid, AC; atypical carcinoid, sclc; small cell lung cancer, LCLC; large-cell neuroendocrine carcinoma, FLT4; Fms-related tyrosine kinase 4, FIGF; C-fos-induced growth factor.
Probe sets for each gene in the CodeSet were designed and synthesized at NanoString Technologies, Seattle, USA. Total RNA (100ng) including miRNA from FFPE material was measured at the NanoString nCounter Core Facility at the University of Heidelberg, Germany.
NanoString Data Processing and Statistical Analysis
Raw NanoString counts for each gene were subjected to a technical normalization considering the counts obtained for positive control probe sets. After the technical normalization, a biological normalization using the three reference genes included in the CodeSet was performed.
All statistical analyses were performed with the R statistical programming environment (v2.15.2). For dichotomous factors such as gender and expression level the Wilcoxon Mann-Whitney rank sum test was applied. For variables with more than two categories the Kruskal-Wallis test was performed. Correlations between gene expression of tested genes and correlations between gene expression and TNM-criteria were analysed by Spearman's rank correlation test. Kaplan-Meier analysis was performed to test associations between gene expression and overall survival (OS) and progression-free survival (PFS). PFS was calculated from the first day of platinum-based chemotherapy until progression, death from any cause, or the last time of follow up without progression. OS was defined as the time between the start of platinum-based chemotherapy until the date of death, or last follow-up. Patients were censored at the last follow-up if still alive or lost to follow-up. Surveillance of PFS and OS was stopped on July 31, 2012. Significant differences in PFS or OS between groups were verified by the Wald-test, likelihood-ratio test and Score (logrank) test.
The level of statistical significance was defined as p≤0.05.
Results
The mean age at date of diagnosis was 58.58 years (median age: 58.99 years; 95% CI: 50.79-66.92 months). Survival data was available for 34 patients with eight reported deaths at the time of data collection. Data are summarized in Figs. 2-4.
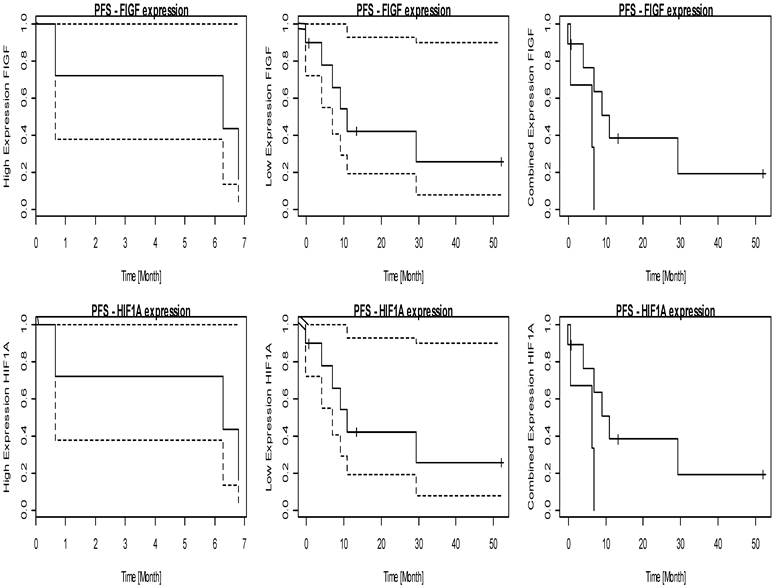
FIGF; C-fos-induced growth factor, HIF1A; Hypoxia-inducible factor 1-alpha.
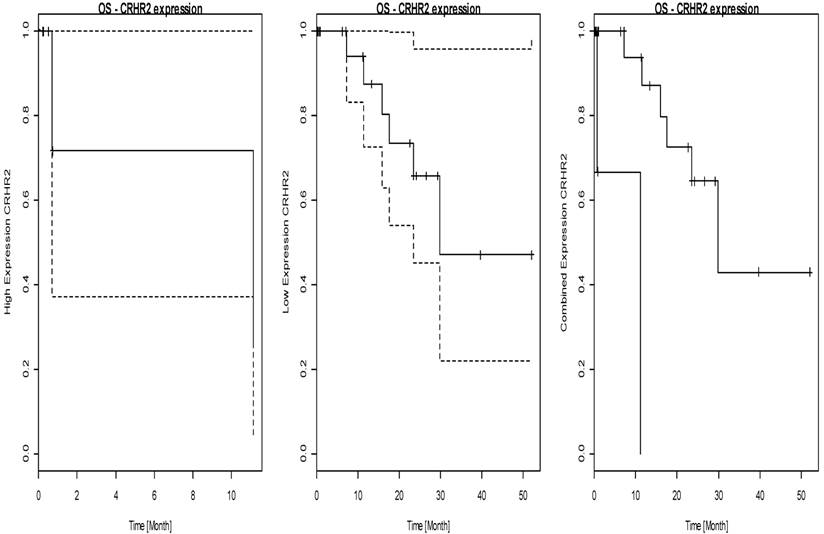
CRHR2; Corticotropin releasing hormone receptor 2.
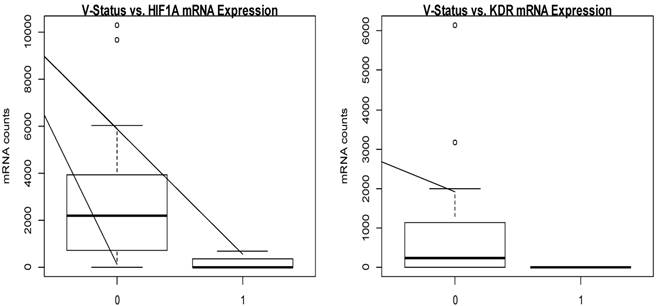
HIF1A; Hypoxia-inducible factor 1-alpha, KDR; Kinase insert domain receptor.
Overall Collective
In the overall collective, FIGF and FLT4 gene expression significantly differs between the investigated entities of neuroendocrine tumours (FIGF: p=0.0096, FLT4: 0.0054). FIGF just shows expression in TC as well as in LCNEC. Expression of FLT4 decreases from TC to SCLC and therefore also shows significant indirect correlation to pathological tumour grade (p=0.0025). Also KDR rendered significant association to aggressiveness of the tumour and decreases with increasing malignancy (p=0.049).
A decreased expression of HIF1A and KDR mRNA as associated with a higher risk of tumour invasion in vessels (HIF1A: p=0.034; KDR: p=0.029).
CRHR2 mRNA expression leading to two separate groups of tumours, thereby high CRHR2 mRNA levels predict dramatically shortened overall survival time in pulmonary neuroendocrine tumours (p= 0.040). Furthermore, FIGF and HIF1A expression levels are significantly associated with progression-free survival (FIGF: p= 0.021; HIF1A: p= 0.049).
CRHR2 and FLT4 are stronger expressed in female than in male patients (CRHR2: p=0.024, FLT4: p=0.004).
Low-Grade Pulmonary Neuroendocrine Tumours (carcinoids)
As FIGF is just expressed in TC and not in AC, FIGF is a highly specific marker to differentiated TC from AC (p=0.003). Within the carcinoid group of tumours, MMP3 is just expressed in G2 and not in G1 tumours (p=0.019).
Like in the overall collective, FLT4 is much higher expressed in women than in men (p=0.006).
High-Grade Pulmonary Neuroendocrine Tumours (carcinomas)
Nevertheless FIGF mRNA expression is not remarkable in this two entities of high-grade tumours, FIGF expression is still significant between LCNEC and SCLC (p=0.023).
LG Versus HG Pulmonary Neuroendocrine Tumours
Between low-grade and high-grade neuroendocrine tumours of the lung, FLT4 and KDR show highly significant association to one of the analysed groups (FLT4: p=0.001; KDR: p=0.006).
Additionally, HIF1A expression differs significantly between these focus cohorts (p=0.018).
Discussion
Tumourigenesis and cancer proliferation has been known to be closely associated with angiogenesis in lung cancer [23]. The following pathways have been identified to influence tumour angiogenesis; a) vascular endothelial growth factor165b, b) vascular endothelial growth factor-A, c) interleukin 1β and d) tumour transforming factor (TGF)-1β [24]. The leucocyte and platelet counts have been correlated with the previous factors and clinical outcomes [24]. Currently several imaging techniques have been investigated to demonstrate the angiogenesis level within tumours as an addition to the investigation of several serum circulating factors [25]. These techniques have been found to be useful both at the preclinical and the clinical setting. In squamous cell carcinoma angiogenesis and mast cell density where positively correlated with each other. Microvessel density (MVD) was also associated with decreased survival, implicating that in squamous cell carcinoma anti-angiogenetic treatment should be included, however; with novel compounds [26]. The polymorphisms of Hypoxia-inducible factor 1-alpha (HIF1A), have been associated with prognosis of early stage non-small-cell lung cancer patients after surgery [27]. The HIF1A was observed to be attenuated by carbon ion radiotherapy, enhancing the therapeutic efficiency of treatment [28]. The main antiangiogenic agent in the first line is bevacizumab, however; recently completed studies have investigated cediranib, sorafenib, motesanib, axitinib and the vascular disrupting agent vadimezan [29]. To date no agents have been approved for the treatment of relapsed/refractory non-small cell lung cancer. There have been several studies targeting the angiogenesis for lung cancer with tyrosine kinase inhibitors (TKIs) (nintedanib, vandetanib, sorafenib, sunitinib), however; without any benefit for overall survival [30-32]. It has been observed that vascular endothelial growth factor receptors-TKIs also inhibit other molecular pathways such as; platelet derived growth factor (PDGFR) and proto-oncogene c-Kit (KIT) [33]. Nintedanib is known to target fibroblast growth factor receptor (FGFR) and therefore increased efficacy has been observed compared to other TKIs. Moreover; nintedanib has been observed to target proto-oncogene tyrosine-protein kinase (Src) and cluster of differentiation antigen 135 (CD135) [34]. Furthermore; ramucirumab, cediranib, pazopanib and linifanib have been recently investigated. However; the benefit could not overtake the benefit of nintedanib (triple kinase inhibitor) when added to docetaxel as a second line treatment of patients with adenocarcinoma [35]. The FUS-interacting serine-arginine-rich protein 1 (FUS1) and interleukin-12 have been targeted with a cationic liposome plasmid targeted these two factors. The results indicated an inhibition of VEGF, VEGFR and upregulation of C-X-C motif chemokine 10 (CXCL10) also known as Interferon gamma-induced protein 10 (IP-10). In this case anti-angiogenesis and immunomodulation was induced as anticancer treatment [36]. Again, in another gene therapy investigation another approach towards inhibition of angiogenesis and metastasis with the tumour-specific delivery of histidine-rich glycoprotein was performed with success [37]. Another novel inhibitor that has been investigated is sanguimarine. It has the ability decrease the secretion of VEGF and silmutaneously decrease the expression of human microvascular ebdothelial cells (HMVECs). In another method of gene therapy two novel nucleolin aptamer-siRNA chimeras (aptNCL-SLUGsiR and aptNCL-NRP1siR) were used to block angiogenesis and distal metastasis [38]. Through suppression of SLUG and NRP1 the chimeras synergistically reduced cancer cell motility and invasive ability. Additionally, circulating tumour cells and tumour growth were suppressed. Sanguinarine was also observed to inhibit VEGF-mediated Akt, p38 activation and VE-cadehrin protein phosphorilation [39]. Another dietary supplement the plant phospholipid/lipid conjugate (pPLC) was used as a water soluble formulation and it was observed to reduce by 30% tumour growth in vivo. The pPLC contains antioxidants that also enhanced the expression of hypoxia-related genes pentraxin-3 and metallothionein-3 [40]. Furthermore; the following pathways; a: STAT1 and STAT3 have been investigated as possible targets for blocking angiogenesis. Indeed, STAT1 was blocked with the use of interleukin-27 (IL-27) which also inhibited the epithelial-mesenchymal transition in human non-small cell lung cancer [41]. However; IL-27 had no effect on STAT3 blockage [41]. The STAT3 pathway was observed to be efficiently blocked with dimethylaminoparhenolide (DMAPT) which is a water soluble parthenolide [42]. It was also observed that the drug was more effective against large tumours more >2cm [42]. Another novel drug the DPMA a deoxypodophyllotoxin derivative exhibited superior cytotoxicity compared with etoposide. This agent exhibited anti-proliferative activity and induced apoptosis in lung cancer cells in a dose and time dependent manner [43]. DPMA also inhibits microtubule formation and induces expression of p53, cleavage caspace-3, Bax, Bcl-2 and reactive oxidative stress proteins (ROS) [43]. In our study we investigated the effect of several factors (Corticotropin releasing hormone receptor 2 (CRHR2), Fms-related tyrosine kinase 4, -fos-induced growth factor (FIGF), tC-fos-induced growth factor (FIGF), Kinase insert domain receptor (KDR) and Hypoxia-inducible factor 1-alpha (HIF1A)) the environment modulation of carcinoids giving emphasis to angiogenesis. Recently an association between IL-6 levels and non-small adenocarcinoma transformation to small-cell neuroendocrine carcinoma was made with the additional help of p38 MAPK [44]. Novel targets blocking the expression of interleukins are already on the market and others are being tested [44, 45]. These targets should be diffused efficiently within the environment of a solid tumor as in the case of lung cancer. In specific, the following factors should be considered when designing a drug; extracellular matrix, passive transportation or active transportation and method of application (local therapy or systematic) [46-48].
Conclusion
The microenvironment is known not only to induce tumourigenesis, but also to modulate cancer types [44]. We should consider for clinical practice application which factors affect most the tumour growth and distal metastasis, thereafter investigate easy to administer drugs with low side effects. Probably a cluster system of therapy should be established where a drug targets simultaneously different pathways of the same origin.
Conflict of Interest
All authors disclose any affiliations that are considered to be relevant and important with any organization that to our knowledge has any direct interest in the subject matter discussed.
References
1. Eramo A. et al. Identification and expansion of the tumorigenic lung cancer stem cell population. Cell Death Differ. 2008;15(3):504-14
2. Jett J.R. and Midthun D.E. Screening for lung cancer: current status and future directions: Thomas A. Neff lecture. Chest. 2004;125(5 Suppl):158-62
3. Mallick R. et al. MicroRNAs and lung cancer: Biology and applications in diagnosis and prognosis. J Carcinog. 2010 9
4. Rekhtman N. Neuroendocrine tumors of the lung: an update. Arch Pathol Lab Med. 2010;134(11):1628-38
5. Takei H. et al. Large cell neuroendocrine carcinoma of the lung: a clinicopathologic study of eighty-seven cases. J Thorac Cardiovasc Surg. 2002;124(2):285-92
6. Swarts D.R. et al. Molecular and cellular biology of neuroendocrine lung tumors: evidence for separate biological entities. Biochim Biophys Acta. 2012;1826(2):255-71
7. Thomas C.FJr. et al. Typical and atypical pulmonary carcinoids: outcome in patients presenting with regional lymph node involvement. Chest. 2001;119(4):1143-50
8. Travis W.D. et al. Survival analysis of 200 pulmonary neuroendocrine tumors with clarification of criteria for atypical carcinoid and its separation from typical carcinoid. Am J Surg Pathol. 1998;22(8):934-44
9. Asamura H. et al. Neuroendocrine neoplasms of the lung: a prognostic spectrum. J Clin Oncol. 2006;24(1):70-6
10. Cardillo G. et al. Bronchial carcinoid tumors: nodal status and long-term survival after resection. Ann Thorac Surg. 2004;77(5):1781-5
11. Beasley M.B. et al. Pulmonary atypical carcinoid: predictors of survival in 106 cases. Hum Pathol. 2000;31(10):1255-65
12. Fink G. et al. Pulmonary carcinoid: presentation, diagnosis, and outcome in 142 cases in Israel and review of 640 cases from the literature. Chest. 2001;119(6):1647-51
13. Garcia-Yuste M. et al. Typical and atypical carcinoid tumours: analysis of the experience of the Spanish Multi-centric Study of Neuroendocrine Tumours of the Lung. Eur J Cardiothorac Surg. 2007;31(2):192-7
14. Pelosi G. et al. Alteration of the E-cadherin/beta-catenin cell adhesion system is common in pulmonary neuroendocrine tumors and is an independent predictor of lymph node metastasis in atypical carcinoids. Cancer. 2005;103(6):1154-64
15. Rea F. et al. Outcome and surgical strategy in bronchial carcinoid tumors: single institution experience with 252 patients. Eur J Cardiothorac Surg. 2007;31(2):186-91
16. Travis WD. Lung tumours with neuroendocrine differentiation. Eur J Cancer. 2009;45( Suppl 1):251-66
17. Scott WJ. Surgical treatment of other bronchial tumors. Chest Surg Clin N Am. 2003;13(1):111-28
18. Travis WD. et al. Pathology and genetics of tumours of the lung, pleura, thymus and heart; World Health Organization classification of tumours. Lyon Oxford: IARC Press. 2004:344
19. Jagoe R. et al. Observer variation in quantification of immunocytochemistry by image analysis. Histochem J. 1991;23(11-12):541-7
20. Jarlov AE. Observer variation in the diagnosis of thyroid disorders. Criteria for and impact on diagnostic decision-making. Dan Med Bull. 2000;47(5):328-39
21. Travis W.D. et al. Reproducibility of neuroendocrine lung tumor classification. Hum Pathol. 1998;29(3):272-9
22. den Bakker MA. et al. Small cell carcinoma of the lung and large cell neuroendocrine carcinoma interobserver variability. Histopathology. 2010;56(3):356-63
23. Folkman J. Tumor angiogenesis: therapeutic implications. N Engl J Med. 1971;285(21):1182-6
24. Kim JW. et al. Clinical Implications of VEGF, TGF-beta1, and IL-1beta in Patients with Advanced Non-small Cell Lung Cancer. Cancer Res Treat. 2013;45(4):325-33
25. Yip C. et al. Imaging assessment of lung tumor angiogenesis: insights and innovations. Semin Respir Crit Care Med. 2014;35(1):112-28
26. Ullah E, Nagi AH, Ashraf M. Angiogenesis and mast cell density as predictors of patient survival in squamous cell carcinoma of lung. J Cancer Res Ther. 2013;9(4):701-5
27. Liu B. et al. Polymorphisms of HIF1A gene are associated with prognosis of early stage non-small-cell lung cancer patients after surgery. Med Oncol. 2014;31(4):877
28. Subtil FS. et al. Carbon ion radiotherapy of human lung cancer attenuates HIF-1 signaling and acts with considerably enhanced therapeutic efficiency. FASEB J. 2014;28(3):1412-21
29. Crino L, Metro G. Therapeutic options targeting angiogenesis in nonsmall cell lung cancer. Eur Respir Rev. 2014;23(131):79-91
30. Natale RB. et al. Phase III trial of vandetanib compared with erlotinib in patients with previously treated advanced non-small-cell lung cancer. J Clin Oncol. 2011;29(8):1059-66
31. Scagliotti GV. et al. Sunitinib plus erlotinib versus placebo plus erlotinib in patients with previously treated advanced non-small-cell lung cancer: a phase III trial. J Clin Oncol. 2012;30(17):2070-8
32. Herbst RS. et al. Efficacy of bevacizumab plus erlotinib versus erlotinib alone in advanced non-small-cell lung cancer after failure of standard first-line chemotherapy (BeTa): a double-blind, placebo-controlled, phase 3 trial. Lancet. 2011;377(9780):1846-54
33. Scagliotti G, Govindan R. Targeting angiogenesis with multitargeted tyrosine kinase inhibitors in the treatment of non-small cell lung cancer. Oncologist. 2010;15(5):436-46
34. Kutluk CB. et al. BIBF 1120 (nintedanib), a triple angiokinase inhibitor, induces hypoxia but not EMT and blocks progression of preclinical models of lung and pancreatic cancer. Mol Cancer Ther. 2013;12(6):992-1001
35. Reck M. et al. Docetaxel plus nintedanib versus docetaxel plus placebo in patients with previously treated non-small-cell lung cancer (LUME-Lung 1): a phase 3, double-blind, randomised controlled trial. Lancet Oncol. 2014;15(2):143-55
36. Ren J. et al. Cationic Liposome Mediated Delivery of FUS1 and hIL-12 Coexpression Plasmid Demonstrates Enhanced Activity against Human Lung Cancer. Curr Cancer Drug Targets. 2014
37. Cheng X. et al. Tumor-Specific Delivery of Histidine-Rich Glycoprotein Suppresses Tumor Growth and Metastasis by Anti-Angiogenesis and Vessel Normalization. Curr Gene Ther. 2014
38. Lai WY. et al. Synergistic inhibition of lung cancer cell invasion, tumor growth and angiogenesis using aptamer-siRNA chimeras. Biomaterials. 2014;35(9):2905-14
39. Xu JY. et al. Sanguinarine is a novel VEGF inhibitor involved in the suppression of angiogenesis and cell migration. Mol Clin Oncol. 2013;1(2):331-336
40. Shuman MLA. et al. Dietary intake of a plant phospholipid/lipid conjugate reduces lung cancer growth and tumor angiogenesis. Carcinogenesis. 2014
41. Kachroo P. et al. IL-27 inhibits epithelial-mesenchymal transition and angiogenic factor production in a STAT1-dominant pathway in human non-small cell lung cancer. J Exp Clin Cancer Res. 2013;32(1):97
42. Song JM. et al. Dimethylaminoparthenolide, a water soluble parthenolide, suppresses lung tumorigenesis through down-regulating the STAT3 signaling pathway. Curr Cancer Drug Targets. 2014;14(1):59-69
43. Sang CY. et al. DPMA, a deoxypodophyllotoxin derivative, induces apoptosis and anti-angiogenesis in non-small cell lung cancer A549 cells. Bioorg Med Chem Lett. 2013;23(24):6650-5
44. Zarogoulidis P, Yarmus L, Zarogoulidis K. New insights for IL-6 targeted therapy as an adjuvant treatment for non-small-cell lung cancer. Ther Deliv. 2013;4(10):1221-3
45. Dorff TB. et al. Clinical and correlative results of SWOG S0354: a phase II trial of CNTO328 (siltuximab), a monoclonal antibody against interleukin-6, in chemotherapy-pretreated patients with castration-resistant prostate cancer. Clin Cancer Res. 2010;16(11):3028-34
46. Hohenforst-Schmidt W. et al. Intratumoral chemotherapy for lung cancer: re-challenge current targeted therapies. Drug Des Devel Ther. 2013;7:571-83
47. Baliaka A. et al. Intratumoral gene therapy versus intravenous gene therapy for distant metastasis control with 2-diethylaminoethyl-dextran methyl methacrylate copolymer non-viral vector-p53. Gene Ther. 2014;21(2):158-67
48. Zarogoulidis P. et al. Interleukin-6 cytokine: a multifunctional glycoprotein for cancer. Immunome Res. 2013;9(62):16535
Author contact
Corresponding author: Paul Zarogoulidis, Pulmonary Department-Oncology Unit, ``G. Papanikolaou`` General Hospital, Aristotle University of Thessaloniki, Thessaloniki, Greece. Tel: +306977271974, Fax: +302310992433, e-mail: pzarogcom.

 Global reach, higher impact
Global reach, higher impact