Impact Factor ISSN: 1837-9664
J Cancer 2019; 10(14):3232-3238. doi:10.7150/jca.30159 This issue Cite
Research Paper
The mediating role of extent of resection in the relationship between the tumor characteristics and survival outcome of glioma
1. School of Public Health, Guangzhou Medical University, Guangzhou, China
2. Department of Neurosurgery/Neuro-oncology, Sun Yat-Sen University Cancer Center, State Key Laboratory of Oncology in South China, Collaborative Innovation Center for Cancer Medicine, Guangzhou, China
3. College of information science and technology, Jinan University, Guangzhou, China
* These authors contributed equally to this work.
Received 2018-9-24; Accepted 2019-4-26; Published 2019-6-2
Abstract
The prognostic value of tumor characteristics for glioma has been controversial, partly because of a lack of knowledge about how these associations develop. Extent of resection may be factors that mediate the relationship between tumor characteristics and the hazard of death from glioma.
Patients and Methods: This consecutive study retrospectively included a group of 393 treatment-naive patients with newly, pathologically confirmed glioma between January 2004 and December 2014. Information on patient age, gender, Karnofsky Performance Status (KPS), tumor grade, tumor size, tumor location, presence or absence of contrast enhancement on MRI and extent of tumor resection have all been collected. The discrete-time survival model integrating survival outcomes within structural equation models was employed to develop and evaluate a comprehensive hypothesis regarding the direct and indirect impact of tumor characteristics on the hazard of death from glioma, mediated by the extent of resection.
Results: Except for tumor location, the indirect effects of tumor grade, contrast enhancement, and tumor size on PFS of glioma through extent of resection were found significant in the model.
Conclusion: This study provides a better understanding of the process through which tumor characteristics is associated with hazard of death from glioma.
Keywords: Glioma, survival outcome, extent of resection, discrete-time survival model, structural equation model
1. Introduction
Gliomas are the most common type of primary malignant brain tumor1-2, accounting for nearly 80% of the cases3. The treatment modalities for glioma generally encompass of surgical resection, followed by adjuvant chemotherapy and radiotherapy 4-5. Despite aggressive multimodal treatment regimens, the survival of patients with glioma remains dismal6-7, mainly due to its inevitable progression and relapse after initial treatment2, 8-9.
Frequently reported determinants of tumor-related outcomes for glioma patients include patient related factors, such as age10-11 and performance status12, and tumor-related characteristics, such as histopathological characteristics2,11, tumor size13-16 and location16-18. Although there are some evidences supporting the significant associations between tumor characteristics and the survival of gliomas, most studies failed to find any relation. The prognostic value of tumor characteristics is widely considered controversial19, partly because of a lack of knowledge regarding the mechanisms of how these associations develop.
It is relatively straightforward to figure out how some tumor characteristics influence the hazard of death from glioma. For example, the WHO classification of tumors represents a 'malignancy scale' grading scheme20; low-grade gliomas are characterized by a lack of endothelial proliferation and necrosis21. Contrast enhancement on MRI is a specific radiologic feature, has been thought to imply blood-brain barrier is disturbed by invasive tumor cells and suggest a poorer prognosis for glioma22. Larger tumors may have an increasing proliferative ability leading to increasing tumor burden, and subsequently worse survival time23. Nevertheless, there may be other factors that mediate the relationship between tumor characteristics and the hazard of death from glioma.
In this study, the extent of resection (EOR) is proposed as a potential mediator in the association between some tumor characteristics and the hazard of death from glioma. Recent researches emphasize the importance of EOR for survival of glioma 3, 6, 24; maximal safe resection is considered effective to significantly improve survival of gliomas 3, 9. Glioma is known for its infiltrative property; however it is difficult to distinguish the tumor tissue from adjacent normal brain tissue25. Complete resection has been found to be more likely to be achieved in patients with more favorable tumor characteristics26, such as lack of contrast enhancement and smaller tumor size26-27. The glioblastoma multiform (GBM) lesions tend to be irregular in shape and usually include cystic areas, which leads to a lower probability of achieving gross total resection (GTR) 15. Because neurosurgery may not be always feasible because of some tumor locations, it is more likely that GTR be achieved in supratentorial if compared to infratentorial tumors28. As a consequence, residual tumor cell dissemination beyond the margins of resection and resistance to conventional adjuvant therapies lead to the inevitable relapse and increasing hazard of death of glioma29. Whether tumor characteristics plays an indirect role in gliomas survival through the extent of surgical resection remains to be seen.
Given the significant associations between tumor characteristics, extent of resection, the progression (relapse) and outcome (death) of glioma, it is reasonable to hypothesize the extent of resection may mediate the relationship between tumor characteristics and the hazard of death from glioma. However, to the best of our knowledge, no study has investigated this relation. And it is difficult to estimate the indirect effects using conventional survival model such as Cox regression 30-31. In this study, the discrete-time survival model integrated with the survival outcomes within structural equation models30, 32 was employed to develop and test a more comprehensive hypothesis regarding the direct and indirect roles of tumor characteristics on the hazard of death from glioma, mediated by the extent of resection.
2. Patients and Methods
2.1 Study population
This consecutive study retrospectively included a group of 421 treatment-naive patients with newly and pathologically confirmed glioma between January 2004 and December 2014. Patients who had prior history of malignancy or second primary tumor, acute infection or autoimmune diseases, or patients with perioperative surgery-related mortality have been excluded. Clinical information was collected at baseline and regularly updated through follow up. Finally, 28 of these 421 patients have been excluded according to the enrollment criteria, and 393 patients with adequate clinical information were eligible for this study.
2.2 Data collection
Information on patient age, gender, Karnofsky Performance Status (KPS), tumor grade, tumor size, tumor location, presence or absence of contrast enhancement on MRI and extent of tumor resection were collected. The tumor grade of glioma was determined on pathological specimens according to World Health Organization (WHO) international histological classification of central nervous (CNS) tumors20. Gliomas with WHO grade I and II were classified as low grade gliomas, whereas gliomas with grade III and IV were classified as high grade gliomas. Pretreatment contrast-enhanced MRI was performed to obtain the tumor size (the maximum diameter of the glioma) and the presence or absence of contrast enhancement on MRI. Tumor location was categorized as supratentorial and infratentorial areas. The extent of tumor resection was assessed by neurosurgeons according to postoperative MRI. The extent of resection was classified as gross total resection (GTR) or sub-total resection (STR).
Chemotherapy and radiotherapy were recommended as adjuvant therapies after primary tumor resection surgery. Due to economic and general condition reason, a portion of these 393 patients did not receive adjuvant therapy.
Repetitive MRI scan was regularly recommended to study patients, and the information on relapse and survival was updated semiannually through follow-up. Relapse was identified according to latest radiographic evidence. Patients were followed until death or censoring at the end of the study (October 2015). Progression-free survival (PFS) was defined as the time from diagnosis to relapse, death from glioma, or the date of the last follow-up visit.
2.3 Ethical statement
All patients of this study have been provided written informed consent. This study was conducted with the approval of the medical ethics committees, and in accordance with the principles of the Declaration of Helsinki.
2.4 Model specification
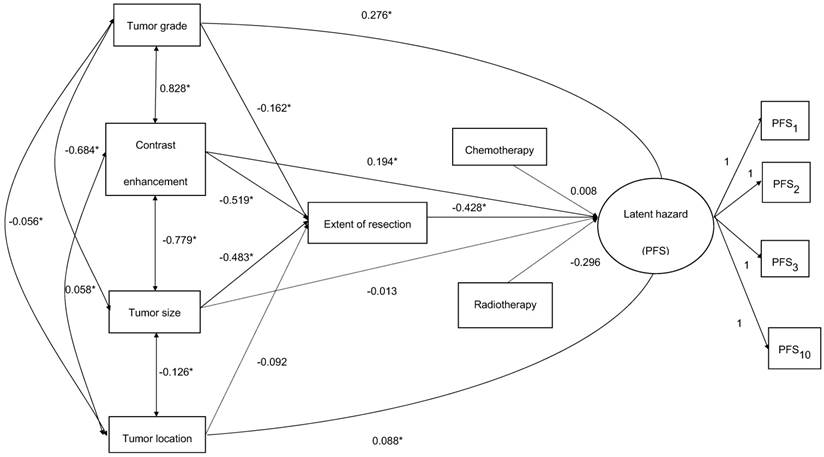
A hypothesis was established that characteristics of glioma such as tumor grade, tumor size, tumor location, and contrast enhancement may influence the extent of resection. And tumor characteristics, the extent of resection, and radiotherapy and chemotherapy have a direct impact on the survival of glioma. And the indirect effect of tumor characteristics on PFS of glioma through extent of resection was explored, as shown in Fig. 1.
Model structure of tumor characteristics on PFS of glioma*P<0.05; dashed represents a non -significant relationship.
2.5 Statistical analyses
Data analyses were performed using the SPSS 21.0 (IBM, Chicago) and Mplus 7.4 (Muthén & Muthén, Los Angeles) software package. In this study, time-to-event data for glioma relapse or death was modeled using a discrete-time survival model, the relapse or survival time was measured continuously before being subsequently transformed into discrete annual intervals. A series of patients with pathologically confirmed and treatment-naive glioma between January 2004 and December 2014 was followed up till October 2015 in this study. This implied a minimum of 1 and a maximum of 12 annual intervals have been observed in our study, and we truncated at 10 as the number of death per year turned negligible after this point.
The latent hazard variable underlying 10 binary time-specific event indicators was described in right part of Fig. 1. Each event indicator had a value of 1 if it (relapse or death for PFS) occurred during this time period and 0 if otherwise. The remaining event indicators were encoded as missing once the event occurred or the patient was lost to follow-up. Ages, genders and KPSs of all patients were included in the model as covariates. The model was analyzed using Maximum Likelihood estimator, and the standard errors (SE) for the indirect effects were estimated using the delta method30.
3. Results
3.1 Patient characteristics and survival outcome
The characteristics of study patients were presented in Table 1. The majority of these patients were males (58.8%), aged less than 60 years (86.8%), had a KPS score larger than 80 (82.7%). According to WHO international histological classification of central nervous (CNS) tumors, 251 (63.9%) of the patients were diagnosed with high grade gliomas (WHO grade III and IV). Tumor size was less than 5 cm in 289 (73.5%) patients. Tumor location was categorized as supratentorial areas in 359 (91.3%) patients, and infratentorial areas in 34 (8.7%) patients. The presence of contrast enhancement on MRI was observed in 336 (85.4%) patients. GTR was achieved in 285 (72.5%) patients. Adjuvant chemotherapy was undertaken in 132 (33.6%) patients, and adjuvant radiotherapy was undertaken in 174 (44.3%) patients.
Characteristics of study patients
| Variable | Number | % |
|---|---|---|
| Gender | ||
| Males | 231 | 58.8 |
| Females | 162 | 41.2 |
| Age group (years) | ||
| ≤60 | 341 | 86.8 |
| >60 | 52 | 13.2 |
| KPS | ||
| ≤80 | 68 | 17.3 |
| >80 | 325 | 82.7 |
| WHO grade | ||
| I/II | 142 | 36.1 |
| III/IV | 251 | 63.9 |
| Tumor Size (cm) | ||
| ≤5 | 289 | 73.5 |
| >5 | 104 | 26.5 |
| Tumor Location | ||
| Supratentorial | 359 | 91.3 |
| Infratentorial | 34 | 8.7 |
| Contrast enhancement on MRI | ||
| Yes | 336 | 85.4 |
| No | 57 | 14.6 |
| Extent of resection | ||
| GTR | 285 | 72.5 |
| STR | 108 | 27.5 |
| Chemotherapy | ||
| Yes | 132 | 33.6 |
| No | 261 | 66.4 |
| Radiotherapy | ||
| Yes | 174 | 44.3 |
| No | 219 | 55.7 |
By the end of the study period, 215 (54.7%) patients had died. The median OS of all the patients was 18.0 months, and the median PFS was 8.3 months.
3.2 Discrete-time survival model (Fig. 1)
3.2.1 Direct effects
The model suggests a significant direct effect of tumor characteristics on PFS of glioma. The direct path coefficients were marked in Fig. 1 and relevant information were shown in Table 2. The model indicated that high grade glioma has led to a substantial increase in the hazard of 0.276 SD (compare to low grade glioma). The presence of contrast enhancement led to an increase in the hazard of 0.194 SD, having glioma sited in infratentorial areas (0.088 SD) rather than supratentorial areas were independently and directly associated with increased hazard. GTR reduced the hazard considerably (-0.428 SD, compare to STR).
The direct and indirect effect of tumor characteristics on PFS of glioma (Fig. 1)
| Variable | Estimated effect | S.E. | Est./S.E. | p-value |
|---|---|---|---|---|
| Direct effects | ||||
| Hazard of death due to glioma (PFS) | ||||
| Tumor grade (III+IV/I+II) | 0.276 | 0.064 | 4.315 | <0.001 |
| Contrast enhancement (Yes/No) | 0.194 | 0.059 | 3.304 | 0.001 |
| Tumor size (>5cm/≤5cm) | -0.013 | 0.049 | -0.273 | 0.785 |
| Tumor location (Infratentorial/Supratentorial) | 0.088 | 0.024 | 3.659 | <0.001 |
| Extent of resection (GTR/STR) | -0.428 | 0.060 | -7.177 | <0.001 |
| Chemotherapy (Yes/No) | 0.008 | 0.029 | 0.293 | 0.769 |
| Radiotherapy (Yes/No) | -0.296 | 0.178 | -1.663 | 0.096 |
| Age | 0.547 | 0.069 | 7.949 | <0.001 |
| Gender (Male/Female) | -0.018 | 0.034 | -0.533 | 0.594 |
| KPS | -0.036 | 0.061 | -0.598 | 0.550 |
| Extent of resection (PFS) | ||||
| Tumor grade (III+IV/I+II) | -0.162 | 0.080 | -2.009 | 0.045 |
| Contrast enhancement (Yes/No) | -0.519 | 0.088 | -5.883 | <0.001 |
| Tumor size (>5cm/≤5cm) | -0.483 | 0.084 | -5.763 | <0.001 |
| Tumor location (Infratentorial/Supratentorial) | -0.092 | 0.074 | -1.244 | 0.213 |
| Age | -0.061 | 0.063 | -0.983 | 0.325 |
| Gender (Male/Female) | 0.033 | 0.050 | 0.662 | 0.508 |
| KPS | -0.325 | 0.074 | -4.390 | <0.001 |
| Indirect effects | ||||
| Tumor grade→Extent of resection→Latent hazard (PFS) | 0.069 | 0.036 | 1.911 | 0.056 |
| Contrast enhancement→Extent of resection→Latent hazard (PFS) | 0.222 | 0.051 | 4.325 | <0.001 |
| Tumor size→Extent of resection→Latent hazard (PFS) | 0.207 | 0.048 | 4.308 | <0.001 |
| Tumor location→Extent of resection→Latent hazard (PFS) | 0.039 | 0.032 | 1.216 | 0.224 |
High grade glioma (-0.162SD) had a lower probability of achieving GTR when compared against its low grade counterpart. The presence of contrast enhancement led to a decrease of 0.519 SD in the probability of achieving GTR. In addition, larger tumor size lower the probability of GTR (-0.483 SD).
3.2.2 Indirect effects
The indirect effects of tumor characteristics on PFS of glioma through extent of resection were shown in Table 2. High grade glioma, the presence of contrast enhancement, large tumor size indirectly increased the hazard by reducing the extent of resection. The indirect effect suggested that the presence of contrast enhancement was significantly associated with an increase in the hazard of 0.222 SD through extent of resection. In addition to the substantial direct effect of contrast enhancement on PFS of glioma, there was indirect effect that account for more than half of the total effect (53.4%).
4. Discussion
A structural equation model with a discrete-time survival outcome was used to estimate both the direct effects of tumor characteristics on hazard of death from glioma and the mediating effects of extent of resection in this study. Finding of this study provided a better understanding of the process through which tumor characteristics are associated with hazard of death from glioma.
In the model, high-grade glioma, the presence of contrast enhancement, and infratentorial glioma were found associated with increased hazard directly. Previous studies reported the associations between these tumor characteristics and the survival of glioma using routine survival analysis method (Log-rank test or Cox regression) 11-13, 16. However, the direct and indirect effect paths have not been depicted in existing studies and inter-associations between different tumor characteristics have not been taken into account. The significant inter-relations among tumor grade, contrast enhancement, tumor location and tumor size were also found in this study.
Although there were studies suggesting the role of extent of resection in the process through which tumor characteristics were associated with the hazard of death from glioma26, no previous study had proven these assumptions using proper statistical models. This study provides concrete evidence that high-grade glioma, contrast enhancement and large tumor size have an indirect influence on the hazard of death from glioma, and that the extent of resection's role as the mediator. Extent of resection in glioma of surgery significantly contributes to an increasing hazard of death caused by unfavorable tumor characteristics. Previous studies have suggested that the contrast enhancement and larger tumor size may influence the extent of resection26-27, and that the extent of resection as an important predictor for relapse and survival of glioma. Although it is not difficult to analyze these relationships separately in common statistical methods (logistic regression, Cox regression), the possible effect pathway among these factors cannot be explored integrally without newly suitable statistical model. Besides the essential direct effect, contrast enhancement was found to have a strong indirect effect on the hazard of death from glioma through the extent of resection. Larger contrast enhancement areas tend to cause more damages to normal brain tissues and immature blood vessels. Previous study found tumors with small contrast enhancing area showed lower ratios of necrosis, and were more likely to undergo GTR26. PFS of glioma could be improved by increasing the extent of resection for tumors with contrast enhancement.
In this study, linear probability model was used for the equation in which the mediator (extent of resection) is the dependent variables30. The estimated R-square for extent of resection is 29.4% in this model, which means 29.4% of the variance of extent of resection explained by tumor characteristics be analyzed. However, the R-square for survival outcome is not defined in this model, because the residual variance is zero for categorical latent hazard variable. Although it is difficult to estimate the degree of determination of tumor characteristics to the survival outcome, the R-square value for extent of resection was not very high. As the survival outcome was highly determined by the extent of resection, there might exist some possible improvable determinants, which could hopefully improve the extent of resection and so as to the survival outcome. More possibly improvable determinants for the extent of resection in addition to the tumor characteristics are probably beyond the scope of this paper but will definitely be explored in our future studies. Several recent studies have analyzed the relationship between IDH1 status/extent of resection and survival and have shown that patients with negative IDH1 benefit less from surgery33-34. Therefore, molecular markers such as IDH mutation status, 1p/19q mutation status, and MGMT methylation should be included in the model in future analyses.
The models used in this study provided us a method to take a closer look at the mediation effect related to survival of glioma, and yielded more refined and powerful explanation regarding the relation between prognostic factors and survival of glioma.
However, it is worth noting that there are still some issues not covered in our study. Firstly, the moderate sample size of our study suggests that some selection bias may exist. However, the data collection on such a sample size for survival of glioma is by no means easy and valuable information has been unveiled from this data set. Secondly, information of PFS might not be accurate, quantification of PFS is very difficult to obtain. Thirdly, the generalization in this study may not be concurrent with that of other studies. Future large longitudinal studies should be conducted to increase the generalizability of this study.
In this study, the indirect effects of tumor characteristics on survival of glioma through the extent of resection were found to be statistically significant and substantial in size. It reminds us that there is a risk of underestimating the comprehensive impact of tumor characteristics on survival outcome if the direct effects are solely focused. Instead of replicating analyses of the associations between prognostic factors and survival outcome of glioma in an endless series of samples, this approach encourages the progressive enrichment of an explanatory model.
Conclusion
Extent of resection may be the factor that mediates the relation between tumor characteristics and the hazard of death from glioma. A lack of knowledge or understanding of the mediation effects may lead to a neglect of the influence of certain variables and impede a full appreciation of their role in determining outcomes. The findings of this study provide a better understanding of the process through which tumor characteristics are associated with hazard of death from glioma.
Acknowledgements
This study was supported by National Natural Science Fund project (NSFC-81703299), Guangdong Provincial Natural Science Fund project (2017A030310274), Project for Outstanding Young Innovative Talents in Colleges and Universities of Guangdong Province (2016KQNCX138).
Competing Interests
The authors have declared that no competing interest exists.
References
1. Baumert BG, Hegi ME, van den Bent MJ. et al. Temozolomide chemotherapy versus radiotherapy in high-risk low-grade glioma (EORTC 22033-26033): a randomised, open-label, phase 3 intergroup study. Lancet Oncol. 2016;17:1521-1532
2. Omuro A, DeAngelis LM. Glioblastoma and Other Malignant Gliomas: A Clinical Review. JAMA. 2013;310(17):1842-1850
3. Almenawer SA, Badhiwala JH, Alhazzani W. et al. Biopsy versus partial versus gross total resection in older patients with high-grade glioma: a systematic review and meta-analysis. Neuro Oncol. 2015;17(6):868-881
4. Wick W, Platten M, Meisner C. et al. Temozolomide chemotherapy alone versus radiotherapy alone for malignant astrocytoma in the elderly: the NOA-08 randomised, phase 3 trial. Lancet Oncol. 2012;13(7):707-715
5. Malmstrom A, Gronberg BH, Marosi C. et al. Temozolomide versus standard 6-week radiotherapy versus hypofractionated radiotherapy in patients older than 60 years with glioblastoma: the Nordic randomised, phase 3 trial. Lancet Oncol. 2012;13(9):916-926
6. He ZQ, Ke C, Al-Nahari F. et al. Low preoperative prognostic nutritional index predicts poor survival in patients with newly diagnosed high-grade gliomas. J Neurooncol. 2017;132:239-247
7. Hervey-Jumper SL, Berger MS. Role of Surgical Resection in Low- and High-Grade Gliomas. Curr Treat Options Neurol. 2014;16:284
8. Perrini P, Gambacciani C, Weiss A. et al. Survival outcomes following repeat surgery for recurrent glioblastoma: a single-center retrospective analysis. J Neurooncol. 2017;131:585-591
9. Chan DT, Hsieh SY, Lau CK. et al. Ten-year review of survival and management of malignant glioma in Hong Kong. Hong Kong Med J. 2017;23:134-139
10. Kita D, Ciernik IF, Vaccarella S. et al. Age as a predictive factor in glioblastomas: population-based study. Neuroepidemiology. 2009;33(1):17-22
11. Krishnatry R, Zhukova N, Guerreiro Stucklin AS. et al. Clinical and Treatment Factors Determining Long-Term Outcomes for Adult Survivors of Childhood Low-Grade Glioma: A Population-Based Study. Cancer. 2016;122(8):1261-1269
12. Wick W, Meisner C, Hentschel B. et al. Prognostic or predictive value of MGMT promoter methylation in gliomas depends on IDH1 mutation. Neurology. 2013;81(17):1515-1522
13. Rapp M, Baernreuther J, Turowski B, Steiger HJ, Sabel M, Kamp MA. Recurrence Pattern Analysis of Primary Glioblastoma. World Neurosurg. 2017;103:733-740
14. Chen MH, Lu C, Sun J. et al. Diagnostic and prognostic value of serum vitronectin levels in human glioma. J Neurol Sci. 2016;371:54-59
15. Wang MY, Cheng JL, Han YH, Li YL, Dai JP, Shi DP. Measurement of tumor size in adult glioblastoma: Classical cross-sectional criteria on 2D MRI or volumetric criteria on high resolution 3D MRI. Eur J Radiol. 2012;81(9):2370-2374
16. Chaichana KL, McGirt MJ, Laterra J, Olivi A, Quinones-Hinojosa A. Recurrence and malignant degeneration after resection of adult hemispheric low-grade gliomas. J Neurosurg. 2010;112(1):10-17
17. Jung TY, Jung S, Moon JH, Kim IY, Moon KS, Jang WY. Early prognostic factors related to progression and malignant transformation of low-grade gliomas. Clin Neurol Neurosurg. 2011;113(9):752-757
18. Aizer AA, Ancukiewicz M, Nguyen PL. et al. Natural history and role of radiation in patients with supratentorial and infratentorial WHO grade II ependymomas: results from a population-based study. J Neurooncol. 2013;115(3):411-419
19. Zhang J, Chen YS, Li YP. et al. Postoperative functional status in patients with supratentorial superficial low-grade glioma. World J Surg Oncol. 2017;15(1):186
20. Louis DN, Ohgaki H, Wiestler OD. et al. The 2007 WHO classification of tumors of the central nervous system. Acta Neuropathol. 2007;114:97-109
21. Babu R, Bagley JH, Park JG, Friedman AH, Adamson C. Low grade astrocytomas: the prognostic value of fibrillary, gemistocytic, and protoplasmic tumor histology. J Neurosurg. 2013;119(2):434-441
22. Sankar T, Moore NZ, Johnson J. et al. Magnetic resonance imaging volumetric assessment of the extent of contrast enhancement and resection in oligodendroglial tumors. J Neurosurg. 2012;116(6):1172-1181
23. Chaichana KL, Chaichana KK, Olivi A. et al. Surgical outcomes for older patients with glioblastoma multiform: preoperative factors associated with decreased survival. J Neurosurg. 2011;114(3):587-94
24. Oppenlander ME, Wolf AB, Snyder LA. et al. An extent of resection threshold for recurrent glioblastoma and its risk for neurological morbidity. J Neurosurg. 2014;120(4):846-853
25. Chan DTM, Yi-Pin Sonia H, Poon WS. 5-Aminolevulinic acid fluorescence guided resection of malignant glioma: Hong Kong experience. Asian J Surg. 2018;41(5):467-472
26. Wang Y, Wang K, Wang J. et al. Identifying the association between contrast enhancement pattern, surgical resection, and prognosis in anaplastic glioma patients. Neuroradiology. 2016;58(4):367-74
27. Schomas DA, Laack NN, Rao RD. et al. Intracranial low-grade gliomas in adults: 30-year experience with long-term follow-up at Mayo Clinic. Neuro Oncol. 2009;11(4):437-445
28. Aizer AA, Ancukiewicz M, Nguyen PL. et al. Natural history and role of radiation in patientswith supratentorial and infratentorial WHO grade IIependymomas: results from a population-based study. J Neurooncol. 2013;115(3):411-419
29. Ginzkey C, Eicker SO, Marget M. et al. Increase in tumor size following intratumoral injection of immunostimulatory CpG-containing oligonucleotides in a rat glioma model. Cancer Immunol Immunother. 2010;59(4):541-551
30. Pratschke J, Haase T, Comber H, Sharp L, de Camargo Cancela M, Johnson H. Mechanisms and mediation in survival analysis: towards an integrated analytical framework. BMC Med Res Methodol. 2016;16:27
31. Aalen OO. Armitage lecture 2010: understanding treatment effects: the value of integrating longitudinal data and survival analysis. Stat Med. 2012;31:1903-1917
32. Comber H, Sharp L, de Camargo Cancela M, Haase T, Johnson H, Pratschke J. Causes and outcomes of emergency presentation of rectal cancer. Int J Cancer. 2016;139(5):1031-1039
33. Claus EB, Walsh KM, Wiencke JK. et al. Survival and low-grade glioma: the emergence of genetic information. Neurosurg Focus. 2015;38(1):E6
34. Johnson BE, Mazor T, Hong C. et al. Mutational analysis reveals the origin and therapy-driven evolution of recurrent glioma. Science. 2014;343(6167):189-193
Author contact
Corresponding authors: Wang Jian, Department of Neurosurgery/Neuro-oncology, Sun Yat-sen University Cancer Center; State Key Laboratory of Oncology in South China, Collaborative Innovation Center for Cancer Medicine, No. 651, Dong Feng East Road, Guangzhou 510080, China. E-mail: wangjian_sysucccom; Tel: 86-20-87343656 or Zhu Wei-Heng, College of information science and technology, Jinan university, No 601, Huangpu West Road, Guangzhou 510632, China. E-mail: tzhuwhedu.cn; Tel: 86-20-85220227.

 Global reach, higher impact
Global reach, higher impact