3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(5):1356-1364. doi:10.7150/jca.51972 This issue Cite
Research Paper
Evaluation of diagnostic and predictive values of the serum VEGF-A level and systemic immune-inflammation index in small cell lung cancer
1. Department of Medical Oncology, The First Affiliated Hospital of Bengbu Medical College, Bengbu, Anhui, People's Republic of China.
2. Department of Radiation Oncology, The First Affiliated Hospital of Bengbu Medical College, Bengbu, Anhui, People's Republic of China.
3. Department of Surgical Oncology, The First Affiliated Hospital of Bengbu Medical College, Bengbu, Anhui, People's Republic of China.
4. Department of Clinical Laboratory, The First Affiliated Hospital of Bengbu Medical College, Bengbu, Anhui, People's Republic of China.
*These authors contributed equally to this study.
Abstract
Purpose: To evaluate diagnostic and predictive values of the serum vascular endothelial growth factor-A (VEGF-A) level and systemic immune-inflammation index (SII) in small cell lung cancer (SCLC) patients.
Methods: From January 2018 to April 2020, we prospectively enrolled 59 untreated SCLC patients in the study group and 50 non-neoplastic patients in the control group. Blood samples were collected at baseline, after the first two cycles of chemotherapy and at progression in the study group and at entry in the control group. Serum VEGF-A was measured by chemiluminescence, SII was calculated based on complete blood count results, and the relationship between the VEGF-A/SII and clinicopathological characteristics, chemotherapeutic efficacy and progression-free survival (PFS) of SCLC patients was analyzed.
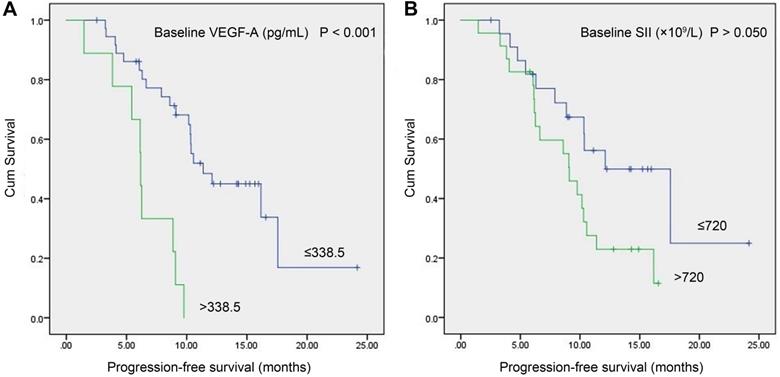
Results: Baseline serum VEGF-A was significantly higher in SCLC patients than in non-neoplastic patients (P<0.001), while baseline SII was not (P=0.114). There was no correlation between baseline VEGF-A and SII in SCLC patients (P=0.123); however, there was a significant correlation between baseline VEGF-A and disease stage and central nervous system (CNS) metastasis (P=0.021 and P=0.012, respectively), as well as between baseline SII and disease stage and liver metastasis (P=0.026 and P=0.018, respectively). Serum VEGF-A was significantly lower than the pretreatment level after 2 cycles of treatment (P=0.049) but was not different at progression (P=0.247). Baseline VEGF-A was correlated with the treatment response of first-line chemotherapy (P=0.001), while baseline SII was not (P=0.392). Kaplan-Meier survival analysis suggested that the PFS of first-line chemotherapy was significantly longer in the low-VEGF-A group at baseline than the high-VEGF-A group (11.37 vs. 6.17 months, P<0.001). There was a trend toward longer PFS of first-line chemotherapy in the low-SII group at baseline than the high-SII group, but the difference was not significant (12.10 vs. 9.10 months, P>0.050). Univariate and multivariate Cox regression analyses suggested that baseline VEGF-A (HR: 3.443, 95% CI: 1.330-8.908, P=0.011) was an independent prognostic factor for PFS in SCLC patients.
Conclusions: Baseline serum VEGF-A and SII are associated with important clinicopathological characteristics of SCLC patients. VEGF-A, but not SII, has the ability of diagnosis and predicting first-line chemotherapeutic efficacy and prognosis in SCLC patients.
Keywords: small cell lung cancer, vascular endothelial growth factor, systemic immune‐inflammation index, diagnosis, prediction, prognosis

 Global reach, higher impact
Global reach, higher impact