Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(12):3427-3438. doi:10.7150/jca.55750 This issue Cite
Research Paper
Computerized Assessment of the Tumor-stromal Ratio and Proposal of a Novel Nomogram for Predicting Survival in Invasive Breast Cancer
1. Hubei Key Laboratory of Tumor Biological Behaviors, Hubei Cancer Clinical Study Center, Wuhan, China, 430071.
2. Department of Gastrointestinal Surgery, Zhongnan Hospital of Wuhan University, Wuhan, China, 430071.
3. Department of Radiology, Zhongnan Hospital of Wuhan University, Wuhan, China, 430071.
4. Department of Radiation and Medical Oncology, Zhongnan Hospital of Wuhan University, Wuhan, China, 430071.
5. Department of Pathology, Renmin Hospital of Wuhan University, 430060 Wuhan, China.
* These authors contribute equally to manuscript.
Abstract
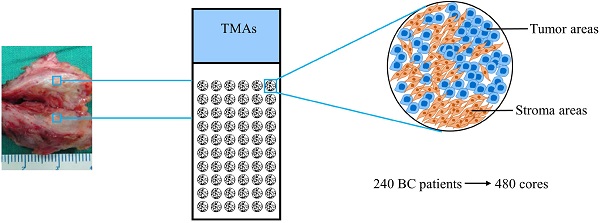
Background: Various studies have verified the prognostic significance of the tumor-stromal ratio (TSR) in several types of carcinomas using manually assessed H&E stained histologic sections. This study aimed to establish a computerized method to assess the TSR in invasive breast cancer (BC) using immunohistochemistry (IHC)-stained tissue microarrays (TMAs), and integrate the TSR into a novel nomogram for predicting survival.
Methods: IHC-staining of cytokeratin (CK) was performed in 7 prepared TMAs containing 240 patients with 480 invasive BC specimens. The ratio of tumor areas and stromal areas was determined by the computerized method, and categorized as stroma-low and stroma-high groups using the X-tile software. The prognostic value of the TSR at 5-year disease free survival (5-DFS) in each subgroup was analyzed. Univariate and multivariate analyses were performed and a novel nomogram for predicting survival in invasive breast cancer was established and assessed.
Results: The newly developed computerized method could accurately recognize CK-labeled tumor areas and non-labeled stromal areas, and automatically calculate the TSR. Stroma-low and stroma-high accounted for 38.8% (n = 93) and 61.2% (n = 147) of the cases, according to the cut-off value of 55.5% for stroma ratio. The Kaplan-Meier analysis showed that patients in the stroma-high group had a worse 5-DFS compared to patients in the stroma-low group (P = 0.031). Multivariable analysis indicated that the T stage, N status, histological grade, ER status, HER-2 gene, and the TSR were potential risk factors of invasive BC patients, which were included into the nomogram (P < 0.10 for all). The nomogram was well calibrated to predict the probability of 5-DFS and the C-index was 0.817, which was higher than any single predictor. A dynamic nomogram was built for convenient use. The area under the curve (AUC) of the nomogram was 0.870, while that of the TNM staging system was 0.723. The Kaplan-Meier analysis showed that the nomogram had a better risk stratification for invasive BC patients than the TNM staging system.
Conclusions: Based on IHC staining of CK on TMAs, this study successfully developed a computerized method for TSR assessment and established a novel nomogram for predicting survival in invasive BC patients.
Keywords: Breast cancer, Tumor stromal ratio, Computerized assessment, Nomogram.

 Global reach, higher impact
Global reach, higher impact