3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(12):3671-3677. doi:10.7150/jca.56170 This issue Cite
Research Paper
Systemic Inflammatory Score predicts Overall Survival in patients with Cervical Cancer
1. Department of Gynecology, Fujian Maternity and Child Health Hospital, Affiliated Hospital of Fujian Medical University, Fuzhou, China.
2. Laboratory of Gynecologic Oncology, Fujian Maternal and Child Health Hospital, Affiliated Hospital of Fujian Medical University, Fuzhou, China.
Abstract
Background: To evaluate the prognostic value of the systemic inflammatory score (SIS) in cervical cancer patients.
Methods: A total of 264 patients with FIGO stage (2009) IB-IIA cervical cancer undergoing radical resection from January 2014 to December 2017 were recruited. The optimal cutoff values for inflammatory biomarkers were calculated by X-tile software. The prognostic factors were investigated using univariate and multivariate Cox analyses. Time-dependent receiver operating characteristic (time-ROC) analysis and the concordance index (C-index) were used to compare the prognostic impact of factors.
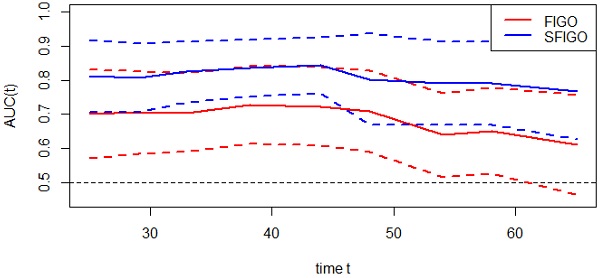
Results: In total, 264 patients with cervical cancer were included in the study. The optimal cutoff value for lymphocyte-to-monocyte ratio (LMR) was 4.1. In multivariate analysis, FIGO stage, lymphovascular invasion, lymph node metastasis, preoperative serum albumin (Alb), and LMR were independent prognostic factors (P<0.05). Then, we combined preoperative Alb and LMR to establish the SIS. Multivariate analysis showed that the SIS was an independent factor that affected survival (P<0.05). When stratified by FIGO stage, significant differences in survival were also found for patients with different SISs (P<0.05). When the SIS and FIGO stage were combined, the time-ROC curve was superior to that of FIGO stage only. The C-index of the model combining the SIS and FIGO stage was 0.786 (95% CI 0.699-0.873), which was significantly higher than that of the model with FIGO stage only (0.676, 95% CI 0.570-0.782, P=0.0049).
Conclusions: The preoperative SIS is a simple and useful prognostic factor for postoperative survival in patients with cervical cancer. It might assist in the identification of high-risk patients among patients with the same FIGO stage.
Keywords: cervical cancer, systemic inflammation score, lymphocyte-to- monocyte ratio, albumin, prognosis

 Global reach, higher impact
Global reach, higher impact