3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2022; 13(2):385-392. doi:10.7150/jca.64800 This issue Cite
Research Paper
The survival impact of palliative radiotherapy on synchronous metastatic pancreatic ductal adenocarcinoma: metastatic site can serve for radiotherapy-decision
1. Department of General Surgery, Xiangya Hospital, Central South University, Changsha, China.
2. National Clinical Research Center for Geriatric Disorders, Xiangya Hospital, Central South University, Changsha, China.
3. Department of Thoracic surgery, Fujian Provincial Hospital, Fuzhou, China.
4. Department of General Visceral and Thoracic Surgery, University Medical Center Hamburg-Eppendorf, Hamburg, Germany.
5. Department of Cardiology, Xiangya Hospital, Central South University, Changsha, China.
6. Department of Rheumatology, Guangdong Provincial People's Hospital, Guangdong Academy of Medical Sciences, Guangzhou, China.
*Co-first authors with equal contributions to this work.
Abstract
Background: The metastatic site seems to represent a malignancy with a different biological characteristic and is an important prognostic factor in metastatic pancreatic ductal adenocarcinoma (mPDAC). Palliative radiotherapy is a therapeutic option, and usually used for pain management in the treatment of mPDAC. The real-world effect of radiotherapy on the survival outcomes of mPDAC patients might do exist and is worth exploring.
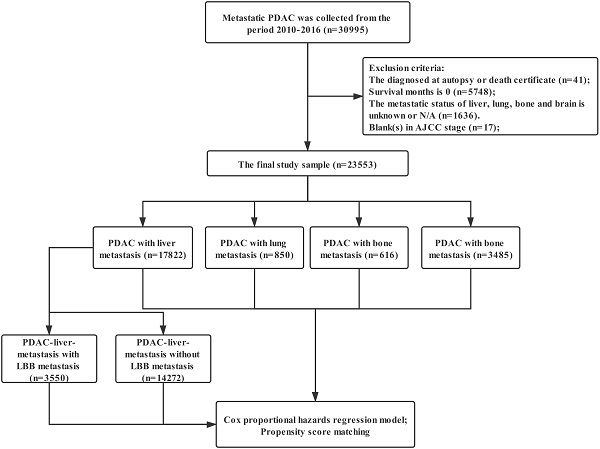
Methods: Data from the Surveillance, Epidemiology, and End Results (SEER) was extracted to identify mPDAC diagnosed in the periods of 2010-2016. The statistical methods included Pearson's chi-square test, Log-rank test, Cox regression model and propensity score matching (PSM).
Results: Radiotherapy was able to improve the overall survival of PDAC with liver metastasis (p<0.001), but not for PDAC patients with lung (p=0.130), bone (p=0.451) and brain metastasis (p=0.226) before PSM. Radiotherapy can only a prognostic factor for PDAC liver metastasis (p=0.001) in the cox regression analysis. The survival curves provided consistent results with cox regression analysis (PDAC with liver metastasis: p=0.023, PDAC with lung metastasis: p=0.528, PDAC with bone metastasis: p=0.210, PDAC with brain metastasis: p=0.106) after PSM. We continue to divided PDAC liver patients into PDAC-liver-metastasis with and without lung, bone, and/or brain (LBB) metastasis. Finally, radiotherapy can be used as a feasible treatment to prolong the overall survival of patients with PDAC liver metastasis without LBB metastasis.
Conclusions: Radiotherapy can be used as a feasible treatment to prolong the overall survival of patients with PDAC liver metastasis without LBB metastasis.
Keywords: PDAC, radiotherapy, metastatic site, overall survival, SEER database

 Global reach, higher impact
Global reach, higher impact