Impact Factor ISSN: 1837-9664
J Cancer 2022; 13(13):3485-3494. doi:10.7150/jca.78004 This issue Cite
Research Paper
What Causes Death in Esophageal Cancer Patients Other Than the Cancer Itself: A Large Population-Based Analysis
1. The First School of Clinical Medicine, Zhejiang Chinese Medical University, Hangzhou, Zhejiang, P. R. China.
2. Department of medical oncology, The First Affiliated Hospital of Zhejiang Chinese Medical University (Zhejiang Provincial Hospital of Traditional Chinese Medicine), Hangzhou, Zhejiang, P. R. China.
3. Department of Science and Education, Quzhou Hospital of Traditional Chinese Medicine, Quzhou, Zhejiang, P. R. China.
4. Department of Science and Education, Quzhou TCM Hospital at the Junction of Four Provinces Affiliated to Zhejiang Chinese Medical University, Quzhou, Zhejiang, P. R. China.
*These authors contributed equally to this work.
Abstract
Background: Researches on noncancer causes of death in patients with esophageal cancer (EC) are not in-depth. The objective of this paper is to broadly and deeply explore the causes of death in patients with EC, especially noncancer causes.
Methods: Information about the demographics, tumor-related characteristics, and causes of death of patients with EC who met the inclusion criteria were extracted from the Surveillance, Epidemiology, and End Results (SEER) database. Calculated standardized mortality ratio (SMR) for all causes of death at different follow-up times and performed subgroup analyses.
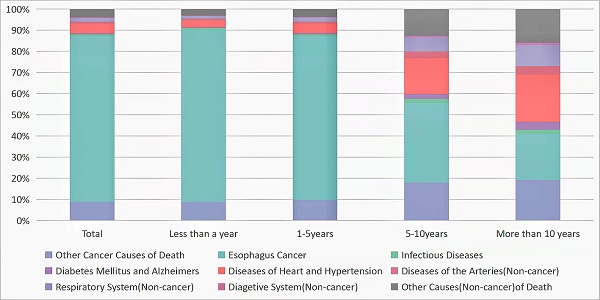
Results: In total, 63,560 patients with EC were retrieved from the public database. And 52,503 died during the follow-up period. Most deaths were due to EC itself within 5 years after diagnosis, but over 10 years, 59% EC patients died from noncancer causes. Cardiovascular disease was the major noncancer cause of death in patients with EC, accounting for 43%. Suicide and self-injury (2%) of EC patients should not be ignored. During the 1-year follow-up period, patients with EC had statistically highest risk of death from septicemia (SMR: 7.61; 95% CI: 6.38-9.00). Within more than 10 years after EC diagnosis, more and more patients died from chronic obstructive pulmonary disease (SMR: 2.38; 95% CI: 1.79-3.10).
Conclusions: Although most patients with EC still died from the cancer itself, the role of noncancer causes of death should not be underestimated. These prompt clinicians to pay more attention to the risk of death caused by these noncancer causes, which can provide relevant measures in advance to intervene.
Keywords: esophageal cancer, noncancer causes of death, standardized mortality ratio, cardiovascular disease, chronic obstructive pulmonary disease, septicemia, suicide and self-injury

 Global reach, higher impact
Global reach, higher impact