3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2023; 14(4):600-610. doi:10.7150/jca.81174 This issue Cite
Research Paper
Clinical Significance of the Combination of Serum HE4 Levels, Hemoglobin-to-Red Cell Distribution Width Ratio, and CT Imaging for the Pretreatment Assessment of Adnexal Masses
1. Department of Obstetrics and Gynecology, Dongsan Medical Center, Keimyung University School of Medicine, Daegu, Republic of Korea.
2. Department of Obstetrics and Gynecology, Hannah Hospital, Busan, Republic of Korea.
3. Department of Internal Medicine, College of Medicine, Kyung Hee University, Seoul, Republic of Korea.
4. Department of Obstetrics and Gynecology, Pusan National University School of Medicine, Biomedical Research Institute and Pusan Cancer Center, Pusan National University Hospital, Republic of Korea.
5. Department of Obstetrics and Gynecology, Cha University, Ilsan Medical Center School of Medicine, Seoul, Republic of Korea.
6. Department of Nursing, Kyungnam College of Information and Technology, Busan, Republic of Korea.
* These authors contributed equally to this work.
Abstract
Background: This study aimed to determine the optimal combination of biomarkers that can predict epithelial ovarian cancer (EOC) and compare the combination with the risk of ovarian malignancy algorithm (ROMA) or Copenhagen index (CPH-I).
Methods: Data from 66 patients with EOC and 599 patients with benign ovarian masses who underwent definitive tissue diagnosis of adnexal masses between January 2017 and March 2021 were analyzed. The Mann-Whitney U test or Kruskal-Wallis test was used for between-group comparisons of medians. Logistic regression was used to establish an EOC predictor model. Area under the curve (AUC) comparisons between models were performed using the Delong nonparametric approach.
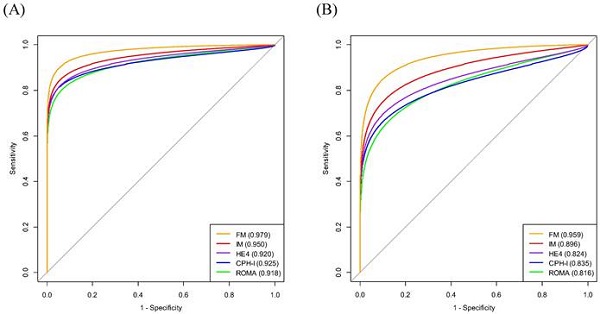
Results: The median age of the patients was 43 years. Twenty-nine (43.9%) patients had early-stage disease (stages I-II) and 37 (56.1%) patients had advanced-stage disease (stages III-IV). The median age, body mass index, white blood cell count, hemoglobin-to-red cell distribution width ratio (HRR), platelet count, platelet-to-lymphocyte ratio, lymphocyte-to-monocyte ratio, serum albumin level, cancer antigen 125, human epididymal secretory protein 4 (HE4), ROMA, and CPH-I were significantly different between the stage I-IV EOC and benign ovarian mass groups. Multivariate logistic regression analysis revealed that HE4, HRR, and computed tomography (CT) imaging were significant predictors of both stages I-IV and I-II EOC. Using these covariates, an interim model (IM) (consisting of HE4 and HRR) and a full model (FM) (consisting of HE4, HRR, and CT imaging) were constructed. When predicting stage I-IV EOC, the AUC of IM was comparable to that of ROMA or CPH-I, whereas the AUC of FM outperformed ROMA or CPH-I. In predicting stage I-II EOC, the AUC of IM was comparable to that of CPH-I but higher than that of ROMA, and the AUC of FM outperformed ROMA or CPH-I.
Conclusion: FM outperformed ROMA or CPH-I in predicting stage I-IV EOC and stage I-II EOC. Therefore, FM could be a promising model for improving preoperative prediction of EOC at an early stage. However, further prospective studies are required to validate these results.
Keywords: HE4 protein, Humans, Red cell distribution width, Computed tomography, Spiral, Adnexal disease.

 Global reach, higher impact
Global reach, higher impact