Impact Factor ISSN: 1837-9664
J Cancer 2021; 12(5):1398-1405. doi:10.7150/jca.51233 This issue Cite
Research Paper
Active Chronic Hepatitis B increases the risk of Colorectal Liver Metastasis - A retrospective cross-sectional study
1. Shandong First Medical University and Shandong Academy of Medical Sciences, 6699 Qingdao road, Huaiyin District, Jinan, China.
2. Department of Hepatobiliary Surgery, Shandong Cancer Hospital and Institute, Shandong First Medical University and Shandong Academy of Medical Sciences, 440 Jiyan road, Huaiyin District, Jinan, China.
3. Department of Oncology, The First Affiliated Hospital of Zhengzhou University, 2 Jianshe East Road, Erqi District, Zhengzhou, China.
4. Department of Hepatobiliary Surgery, The Affiliated Hospital of Qingdao University, 1677 Wutaishan Road, Huangdao District, Qingdao, China.
5. Department of Biostatistics, School of Public Health, Shandong University, 44 Wenhua West Road, Lixia District, Jinan, China.
6. Department of Liver Surgery, Peking Union Medical College Hospital, Chinese Academy of Medical Sciences and Peking Union Medical College, No.1 Shuaifuyuan Wangfujing Dongcheng District, Beijing, China.
7. Department of Surgery, University of Hawaii School of Medicine, 3430 Keahi Place, Honolulu, HI96822, USA.
*These authors contributed equally to this work.
Abstract
Background: A considerable part of colorectal cancer (CRC) patients also have chronic hepatitis B (CHB), esp. in Asia. The effect of concomitant active CHB on the hazard of colorectal liver metastasis (CRLM) remains unclear. To evaluate the effect of concomitant active CHB on the risk of CRLM.
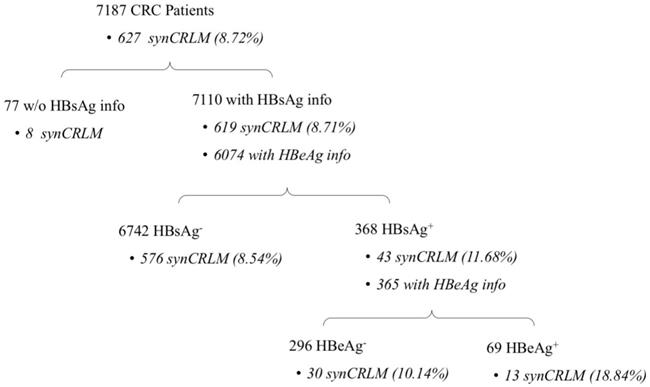
Methods: The medical record of all newly diagnosed CRC patients who were hospitalized to the three hospitals between January 2010 to January 2016 were reviewed, the prevalence of synchronous CRLM (synCRLM) were retrospectively studied. Totally 7187 cases of newly diagnosed CRC, including 368 cases with concomitant CHB were recruited. The prevalence of synCRLM in HBsAg+/HBeAg+ patients was compared to that in HBsAg+/HBeAg- patients. Significant risk factors for synCRLM were analyzed by logistic regression analysis.
Results: The overall prevalence of synCRLM was 8.72% (627/7187) and was significantly higher in HBsAg+ patients (43/368) than HBsAg- patients (576/6742) (11.68% vs. 8.54%, P=0.037; χ2 test).In 368 HBsAg+ patients, 365 patients also had HBeAg information. synCRLM was also more prevalent inHBsAg+/HBeAg+ patients (13/69) compared to HBsAg+/HBeAg- patients (30/296) (18.84% vs. 10.14%, P=0.043; χ2 test). In univariate and multivariate logistic regression analysis, HBeAg positivity was the second strongest predictor of synCRLM (multivariate: OR, 2.622, P=0.020) after CEA. (univariate: OR, 2.920, P=0.001).
Conclusions: HBeAg positivity is a clinical risk factor for CRLM that can be readily identified and addressed. Whether anti-CHB treatment can decrease the risk of CRLM worth carefully-designed prospective trials to define.
Keywords: chronic hepatitis B (CHB), colorectal liver metastasis (CRLM), hepatitis B e antigen (HBeAg), risk

 Global reach, higher impact
Global reach, higher impact