Impact Factor ISSN: 1837-9664
J Cancer 2021; 12(5):1531-1537. doi:10.7150/jca.54617 This issue Cite
Research Paper
Effect of metabolic syndrome components on the risk of malignancy in patients with gallbladder lesions
1. Department of General Surgery, South Campus, Renji Hospital, School of Medicine, Shanghai Jiaotong University, Shanghai, 201112, China
2. Department of Endocrinology, Luwan Branch, Ruijin Hospital, School of Medicine, Shanghai Jiaotong University, Shanghai, 200020, China
3. Department of Gastroenterological Surgery, Tongji Hospital, School of Medicine, Tongji University, Shanghai, 200065, China
4. Department of General Surgery, Changzheng Hospital, The Second Military Medical University, Shanghai, 200003, China
5. Department of Medical Sciences, University of Oxford, Oxford OX3 9DU, United Kingdom
6. Department of General Surgery, Luwan Branch, Ruijin Hospital, School of Medicine, Shanghai Jiaotong University, Shanghai, 200020, China
7. The University of Queensland Diamantina Institute, The University of Queensland, Brisbane, QLD, 4102, Australia
8. Gallipoli Medical Research Institute, Greenslopes Private Hospital, Brisbane, QLD, 4120, Australia
9. Department of biostatistics, clinical research institute, School of Medine, Shanghai Jiaotong University, Shanghai, 200025, China
10. Department of Biliary-Pancreatic Surgery, Renji Hospital, School of Medicine, Shanghai Jiao Tong University, Shanghai, 200127, China
Zheng Deng, Yan Xuan and Xinxing Li contributed equally to this work.
Abstract
Background: Gallbladder lesions have become more common nowadays. But there is limited evidence-based guidance on surveillance of these patients for malignancy. Predicting malignancy could help clinicians better manage this condition and improve the prognosis. We evaluated the independent and joint effects of metabolic syndrome components on the risk of malignancy among patients with gallbladder lesions.
Methods: Using a multicenter database, consecutive patients with pathologically confirmed gallbladder lesions between 2012 and 2019 were identified. Univariate and multivariate logistic regression analyses were used to evaluate the effects of metabolic syndrome components (diabetes, hypertension, dyslipidemia and obesity) as additive or combined indicators for the risk of malignancy. Unadjusted and adjusted odds ratios were calculated.
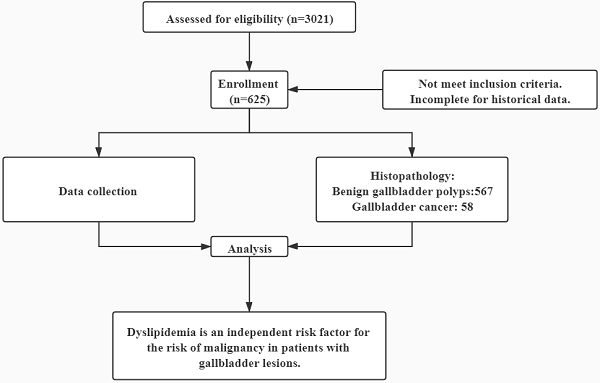
Results: Of the 625 patients, 567 patients were identified with benign gallbladder lesions and 58 patients with gallbladder cancer (GBC). GBC group had less obesity but more dyslipidemia. Among all metabolic syndrome components, only dyslipidemia was significantly associated with GBC (odds ratio 2.674, 95% confidence interval 1.173-6.094). Dyslipidemia was an independent risk factor for malignancy (adjusted odds ratio 2.164, 95% confidence interval 1.165-4.021), regardless of whether the other risk factors and metabolic syndrome components were combined. Patients with decreased high-density lipoprotein had 3.035-fold higher risk of malignancy (adjusted odds ratio 3.035, 95% confidence interval 1.645-5.600).
Conclusions: Dyslipidemia is associated with a 2.674-fold increase in the risk of malignancy in patients with gallbladder lesions. Dyslipidemia is an independent risk factor for malignancy, regardless of the presence of the other risk factors and metabolic syndrome components.
Keywords: Gallbladder lesions, Benign gallbladder polyps, Gallbladder cancer, Metabolic syndrome components, Dyslipidemia, High density lipoprotein

 Global reach, higher impact
Global reach, higher impact