3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(7):2073-2082. doi:10.7150/jca.53198 This issue Cite
Research Paper
Peri-tumoral brain edema associated with glioblastoma correlates with tumor recurrence
1. Department of Neurosurgery, Renmin Hospital of Wuhan University, Wuhan, Hubei 430060, China.
2. John B. Little Center for Radiation Sciences, Department of Environmental Health, Harvard T.H. Chan School of Public Health, Boston, MA 02115, USA.
3. Department of Physiology, School of Basic Medical Sciences, School of Medicine, Wuhan University, Wuhan, Hubei 430071, China.
4. Faculty of Arts and Sciences, Harvard University, Cambridge, MA 02138, USA.
5. Department of Neurology, Renmin Hospital of Wuhan University, Wuhan, Hubei 430060, China.
6. Department of Gynecology and Obstetrics, Renmin Hospital of Wuhan University, Wuhan, Hubei 430060, China.
7. Department of Orthopedics, The First Affiliated Hospital of Jinan University, Guangzhou 510630, China.
8. Department of Biomedical Engineering, Wuhan University School of Basic Medical Sciences, Wuhan, Hubei 430071, China.
9. Department of Geriatrics, Renmin Hospital of Wuhan University, Wuhan, Hubei 430060, China.
* These authors contributed equally to this work.
Abstract
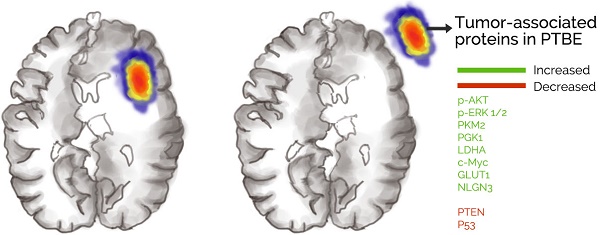
Glioblastoma is the most common malignant tumor of the brain. Despite advances in treatment, the prognosis for the condition has remained poor. Glioblastoma is often associated with peritumoral brain edema (PTBE), which can result in increased intracranial pressure and devastating neurological sequelae if left untreated. Surgery is the main treatment for glioblastoma, however current international surgical guidelines do not specify whether glioblastoma-induced PTBE tissue should be resected. In this study, we analyzed treatment outcomes of PTBE using surgical resection. We performed a retrospective analysis of 255 cases of glioblastoma between 2014 and 2016, and found that a significant proportion of patients had a degree of PTBE. We found that surgical resection led to reduction in midline shift that had resulted from edema, however, postoperative complications and KPS scores were not significantly different in the two conditions. We also observed a delay in glioblastoma recurrence in patients undergoing PTBE tissue resection vs patients without resection of PTBE tissue. Interestingly, there was an abnormal expression of tumor associated genes in PTBE, which has not been previously been found. Taken together, this study indicates that glioblastoma-induced PTBE should be investigated further particularly as the tumor microenvironment is a known therapeutic target and therefore interactions between the microenvironment and PTBE should be explored. This study also highlights the importance of resection of PTBE tissue to not only reduce the mechanical obstruction associated with edema but also to delay recurrence of glioblastoma.
Keywords: Glioblastoma, Peritumoral brain edema, Recurrence, Tumor resection.

 Global reach, higher impact
Global reach, higher impact