3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(14):4418-4423. doi:10.7150/jca.53824 This issue Cite
Research Paper
Efficacy of conversion therapy on initially unresectable locally advanced rectal cancer
1. Colorectal Cancer Center, Department of General Surgery, Zhongshan Hospital, Fudan University, Shanghai, China.
2. Shanghai Engineering Research Center of Colorectal Cancer Minimally Invasive Technology (17DZ2252600), Shanghai, China.
3. Department of Radiotherapy; Zhongshan Hospital, Fudan University, Shanghai, China.
4. Department of Radiology, Zhongshan Hospital, Fudan University, Shanghai, China.
# These authors contributed equally.
Abstract
Background and purpose: Research on the efficacy of conversion therapy for initially unresectable mid-low rectal cancer (IURC) remained limited. This study aimed to assess the efficacy and safety of the conversion regimen for IURC and analyze the long-term outcomes of these patients.
Methods: We retrospectively analyzed the data of clinically diagnosed IURC patients who received conversion therapy between October 2010 and April 2017. The conversion therapy consisted of long-term radiation, concurrent chemotherapy, delayed surgery and consolidation chemotherapy. The primary end point was the rate of R0 resection, and other short- and long-term outcomes were analyzed.
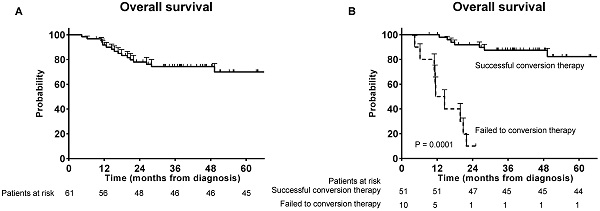
Results: Sixty-one patients were enrolled in this study. After conversion therapy, 51 (83.6%) patients received R0 resection. The rates of pathologic complete response and downstaging were 16.4% and 62.3%, respectively. The rate of grade 3-4 chemoradiotherapy-related toxicity events was 13.1%. The overall survival at 3 years was 75.4% in all patients, and the disease-free survival at 3 years was 72.5% in patients who received R0 resection.
Conclusion: The conversion regimen showed a high conversion resection rate and good survival outcomes in IURC patients, and might benefit the patients if recommended in clinical practice.
Keywords: Unresectable, Rectal Cancer, Conversion Therapy, Prognosis.

 Global reach, higher impact
Global reach, higher impact