Impact Factor ISSN: 1837-9664
J Cancer 2021; 12(15):4488-4496. doi:10.7150/jca.59133 This issue Cite
Research Paper
Pre-treatment high body mass index is associated with poor survival in Asian premenopausal women with localized breast cancer
1. Division of Hematology/Oncology, Department of Internal Medicine, Chang Gung Memorial Hospital, Linkou Branch, Tao-Yuan, Taiwan.
2. Kou Foundation Sun Yat-Sen Cancer Center, Taipei, Taiwan.
3. School of Medicine, Chang Gung University, Tao-Yuan, Taiwan.
4. Department of General Surgery, Chang Gung Memorial Hospital, Linkou Branch, Tao-Yuan, Taiwan.
5. Department of Radiotherapy, Chang Gung Memorial Hospital, Linkou Branch, Tao-Yuan, Taiwan.
Abstract
Background: Obesity is associated with poor prognosis in breast cancer patients. This study aimed to evaluate the effect of obesity measured by body mass index (BMI) on survival of Taiwanese breast cancer patients in a single institution.
Methods: We observed 5000 patients who were diagnosed with stage I-III breast cancer between 1990 and 2005. Information on BMI at diagnosis, and clinical follow-up for disease recurrence and death, up to 20 years post-diagnosis were available. BMI (in kg/m2) categories included normal weight (BMI<24), overweight (24≤BMI<27), and obesity (BMI≥27), according to recommendations from the Bureau of Health Promotion of Taiwan. The role of BMI and other known prognostic factors for patient survival were evaluated in this patient cohort.
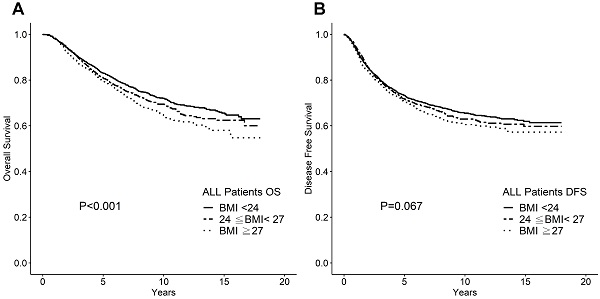
Results: Obesity was associated with advanced stage, higher nuclear grade, and higher percentages of estrogen receptor (ER) positive. The median age of patients with a higher BMI was greater than the median age of patients with a lower BMI. Obesity was an independent prognostic factor of overall survival (OS) (P<0.001), but not disease-free survival (DFS) (P=0.067). We subsequently analyzed the impact of age-stratified BMI (age<50 and age≥50 years) to ameliorate the impact of age bias. Following subset analyses, obesity correlated with shorter DFS (P=0.004) and OS (P=0.009) only in women<50 years of age. Multivariate analysis revealed that BMI was an independent prognostic factor for both DFS and OS in this group of patients. Subset analysis revealed that in women <50 years old, the impact of BMI on survival was associated with higher stage, ER negativity.
Conclusion: BMI is an independent prognostic factor of OS and DFS in breast cancer patients aged<50 years. Although the cause-effect relationship between obesity and survival is unclear, we recommend that weight control measures in young breast cancer survivors should be considered.
Keywords: breast cancer, obesity, prognostic factor, body mass index

 Global reach, higher impact
Global reach, higher impact