Impact Factor
ISSN: 1837-9664
J Cancer 2021; 12(15):4522-4529. doi:10.7150/jca.54650 This issue Cite
Research Paper
Safety and efficacy of drug-eluting bead transarterial chemoembolization with CalliSpheres® microsphere for hepatocellular carcinoma with portal vein tumor thrombus: a preliminary study
1. Hepatobiliary and Pancreatic Interventional Treatment Center, Division of Hepatobiliary and Pancreatic Surgery, The First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang Province, China.
2. Zhejiang Provincial Research Center for Diagnosis and Treatment of Hepatobiliary Diseases, Hangzhou, Zhejiang Province, China.
3. Zhejiang Clinical Research Center of Hepatobiliary and Pancreatic Diseases, Hangzhou 310003, Zhejiang Province, China.
4. Department of Radiology, Jingning County People's Hospital, Lishui, Zhejiang Province, China
5. Department of Radiology, The First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, China.
Abstract
Objective: To prospectively evaluate the safety and therapeutic effectiveness of drug-eluting beads transcatheter arterial chemoembolization (DEB-TACE) with CalliSpheres® microsphere (CSM) for the treatment of hepatocellular carcinoma (HCC) with portal vein tumor thrombus (PVTT), and to analyze the prognostic factors.
Method: Between November 2015 and November 2017, consecutive 58 HCC patients with PVTT who received DEB-TACE with CSM treatment were prospectively enrolled in this study. The demographic characteristics, adverse events (AEs) and treatment response were collected. Overall survival (OS) and progression-free survival (PFS) were calculated using the Kaplan-Meier method. Univariate and multivariate Cox regression analyses were performed to determine the independent factors correlated with OS.
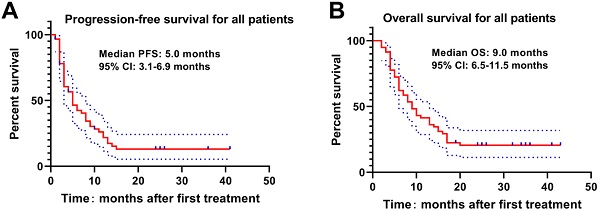
Results: The objective response rate (ORR) was 79.3% in terms of tumors and 44.8% in thrombi. The median PFS and OS of patients were 5.0 months and 9.0 months respectively. The cumulative survival rate at 3-, 6-, 9-, 12-, 18- and 24-month were 94.8%, 72.4%, 53.4%, 41.4%, 22.4% and 19.0%, respectively. In a stepwise multivariate Cox proportional hazards model, the higher Child-Pugh classification (HR=2.279; 95%CI, 1.042-4.985, p = 0.039) and tumor burden (p = 0.008) were the significant predictors of poorer OS after adjustment for known risk factors. The most common clinical AEs were postembolization syndrome (PES) and the most prevalent laboratory toxicity was transient liver function damage.
Conclusion: DEB-TACE with CSM is safe and well-tolerated in HCC patients with PVTT, and reveals a favorable preliminary clinical outcome. The higher Child-Pugh classification and liver tumor burden are independent prognostic factors associated with poor survival for HCC patients with PVTT treated by DEB-TACE with CSM.
Keywords: Hepatocellular carcinoma, Chemoembolization, Therapeutic, Microspheres, Prognosis

 Global reach, higher impact
Global reach, higher impact