Impact Factor
ISSN: 1837-9664
J Cancer 2022; 13(4):1160-1167. doi:10.7150/jca.65817 This issue Cite
Research Paper
Impact of operation duration on short-term and long-term prognosis in patients undergoing radical colorectal surgery
1. Department of Anesthesiology, Fudan University Shanghai Cancer Center, Shanghai, China.
2. Department of Cancer Prevention, Fudan University Shanghai Cancer Center, Shanghai, China.
3. Department of Integrated Therapy, Fudan University Shanghai Cancer Center, Shanghai, China.
4. Department of Oncology, Shanghai Medical College, Fudan University, Shanghai, China.
*Co-first authors with equal contributions to this work.
Abstract
Purpose: The objective of this study was to evaluate the impact of operation duration on short- and long-term outcomes of colorectal cancer patients following surgical resection.
Methods: 6224 consecutive patients who underwent radical colorectal surgery were retrospectively assessed and were divided into short operation duration group (SOD) and long operation duration group (LOD) according to the operation duration cutoff value of 110 minutes.
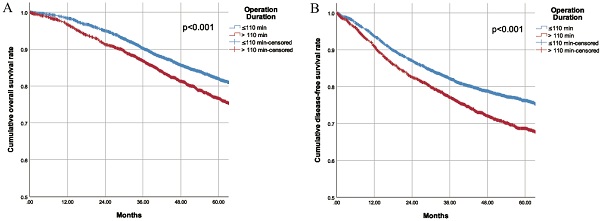
Results: Compared with patients in LOD group, patients in SOD group had significantly lower total costs in hospital, reduced expenses for drugs and antibiotics, shorter length of stay (LOS) in hospital and in the ICU. Moreover, 5-year overall survival (OS) and disease-free survival (DFS) for patients in the SOD group were markedly higher than for patients in the LOD group. Mutivariate regression analysis indicated that longer operation duration was associated with poor prognosis, with a hazard ratio of 1.004 (1.003, 1.005) for OS and 1.005 (1.003, 1.006) for DFS. Finally, surgeons' qualifications had meaningful correlation with operation duration (r= 0.450).
Conclusions: Operation duration is an independent risk factor for patients' short-term and long-term outcome after radical colorectal surgery. Improve the surgical skills of the surgeon may shorten the operation duration, and further improve the outcome for patients.
Keywords: operation duration, short-term and long-term prognosis, colorectal cancer, radical surgery

 Global reach, higher impact
Global reach, higher impact