Impact Factor
ISSN: 1837-9664
J Cancer 2022; 13(5):1565-1572. doi:10.7150/jca.65370 This issue Cite
Research Paper
Next-generation Sequencing Reveals Age-dependent Genetic Underpinnings in Lung adenocarcinoma
1. Department of Medical Oncology, Beijing Hospital, National Center of Gerontology; Institute of Geriatric Medicine, Chinese Academy of Medical Sciences, Beijing, P. R. China
2. Department of Thoracic Medical Oncology, Peking University, School of Oncology, Beijing Cancer Hospital & Institute, Beijing, P. R. China
3. Department of Gerontology, Beijing Hospital, National Center of Gerontology; Institute of Geriatric Medicine, Chinese Academy of Medical Sciences, Beijing, P. R. China
4. Department of Pathology, Beijing Hospital, National Center of Gerontology; Institute of Geriatric Medicine, Chinese Academy of Medical Sciences, Beijing, P. R. China
5. Geneplus-Beijing, Beijing, 102206, P. R. China
6. Geneplus-Shenzhen Genomics Institute, Shenzhen 518000, China
* These authors contributed equally to this work.
Abstract
Background: More than 40% of lung cancer patients are diagnosed at ages over 70. However, the genomic and clinical characteristics among them remain elusive. Here, we performed targeted capture sequence to characterize the mutational spectrum of Chinese lung adenocarcinoma (LUAD) patients across ages.
Patients and Methods: 2025 LUAD patients were divided into three groups: young (≤50 years old) (n=416, 20.54%), intermediate (51~69 years old) (n=1271, 62.77%), and aged (≥70 years old) (n=338, 16.69%). 1,021-gene panel and 59-gene panel were used for sequencing with tissue samples. Genetic alterations and tumor mutation burden (TMB) in LUAD patients were investigated.
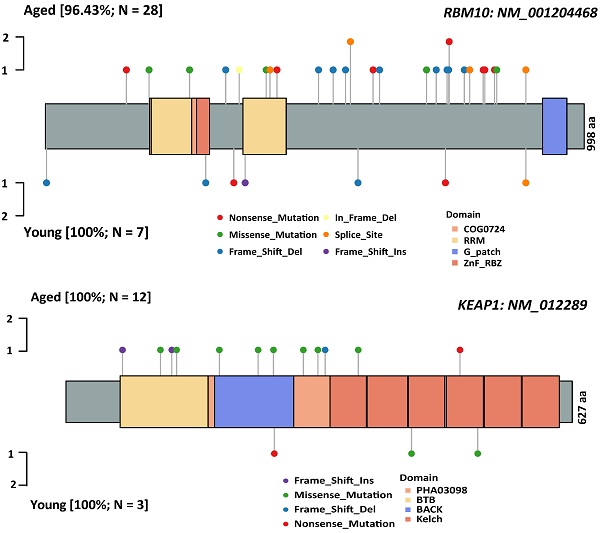
Results: The frequency of mutations affecting 20 genes were significantly higher in aged group than in young group, and fourteen of them were not reported before, including involved in cell cycle/apoptosis signaling (FAT1, FAT2), DNA damage repair (FANCA and FANCM), chromatin histone modification (KDM6A), RTK/RAS/PI3K signaling (FLT4 and MTOR), NOTCH signaling (NOTCH1, NOTCH2 and NOTCH4) and other signaling pathway or cellular regulatory factor (KEAP1, ASXL1, EPHB1 and ABCB1). Six previously reported mutated genes (RBM10, KRAS, LRP1B, CDKN2A and KMT2C/D) were also significantly more frequent in aged group. Among clinical actionable mutation sites, KRAS mutation was presented more common in aged group; both MET exon 14 skipping and MET amplification were significantly positively correlated with old age; the fusions of ALK, ROS1, RET and ERBB2 exon 20 insertion were less frequent in aged group. Furthermore, a higher level of TMB was found in aged group compared with young group.
Conclusion: In this study, we revealed the differences of somatic genetic mutations and TMB between young and aged LUAD patients, which may provide directions of targeted therapy and advantages of immunotherapy for the elderly in the future.
Keywords: Lung adenocarcinoma, Age stratification, Next-generation sequencing, Tumor Mutation Burden.

 Global reach, higher impact
Global reach, higher impact