3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2022; 13(7):2171-2178. doi:10.7150/jca.70894 This issue Cite
Research Paper
The survival impact of radiotherapy on synchronous metastatic rectal cancer: metastatic site can serve for radiotherapy-decision
1. Department of General Surgery, Xiangya Hospital, Central South University, Changsha, China.
2. National Clinical Research Center for Geriatric Disorders, Xiangya Hospital, Central South University, Changsha, China.
3. Department of General Visceral and Thoracic Surgery, University Medical Center Hamburg-Eppendorf, Hamburg, Germany.
4. Department of Thoracic surgery, Fujian Provincial Hospital, Fuzhou, China.
5. Department of Cardiology, Xiangya Hospital, Central South University, Changsha, China.
Abstract
Purpose: The metastatic site seems to represent a malignancy with a different biological characteristic. Radiotherapy, as a successful, well-tolerated, cost-effective and time-efficient intervention, is able to provide clear benefits for the treatment of locally advanced rectal cancer and has become an essential component of palliative oncology care. The real-world effect of radiotherapy on the survival outcomes of metastatic rectal cancer (mRC) patients might do exist and was worth exploring.
Patients and methods: Data were extracted from the Surveillance, Epidemiology, and End Results (SEER) database in this retrospective analysis. The statistical methods included Pearson's chi-square test, Log-rank test, Cox regression model and propensity score matching (PSM).
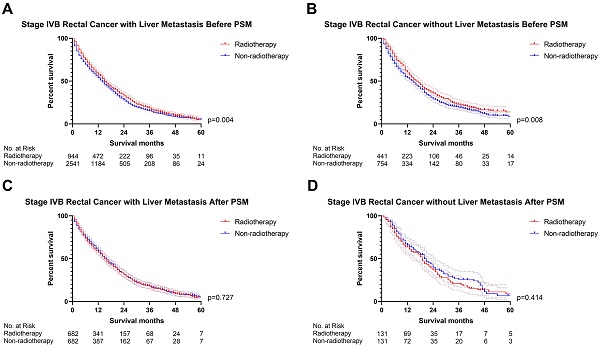
Results: The multivariable Cox regression displayed that radiotherapy may not be used as a prognostic factor for mRC (p=0.057). However, radiotherapy may be associated with the prognosis if the metastatic site was excluded from the multivariate analysis (p<0.001). Radiotherapy seemed to fail to improve OS before PSM (p<0.001) and after PSM without the metastatic site as a matching factor (p<0.001). Nevertheless, there was no significant survival difference between radiotherapy and non-radiotherapy cohort after PSM with the metastatic site as a matching factor (p=0.057). All of M1a rectal cancer patients appear to obtain survival benefit from radiotherapy without the impact of PSM (p<0.001). Notwithstanding, radiotherapy was associated with improved OS of patients with rectal liver-limited metastasis (p=0.023) and did not appear to provide survival benefit for rectal lung-limited (p=0.386) and other-limited metastasis (p=0.385). Both of M1b mRC with and without liver metastasis did not seem to obtain survival benefit from radiotherapy.
Conclusions: Carefully selected data from the SEER database suggested that radiotherapy appears to improve overall survival only in patients with rectal liver-limited metastasis.
Keywords: rectal cancer, radiotherapy, metastatic site, overall survival, SEER database

 Global reach, higher impact
Global reach, higher impact