Impact Factor ISSN: 1837-9664
J Cancer 2022; 13(8):2457-2471. doi:10.7150/jca.63008 This issue Cite
Research Paper
Prognostic Impact of Tumor Budding in Intrahepatic Cholangiocellular Carcinoma
1. Institute of Surgical Pathology, Medical Center - University of Freiburg, Freiburg, Germany
2. Faculty of Medicine, University of Freiburg, Germany
3. Department of Pathology, Memorial Sloan-Kettering Cancer Center, New York, NY, USA
4. German Cancer Consortium (DKTK) and Cancer Research Center (DKFZ), Heidelberg, Germany
5. Tumorbank Comprehensive Cancer Center Freiburg, Medical Center - University of Freiburg, Germany
6. Core Facility for Histopathology and Digital Pathology, Medical Center - University of Freiburg, Freiburg, Germany
7. Clinic of Surgery, UKSH Campus Lübeck, Germany
Abstract
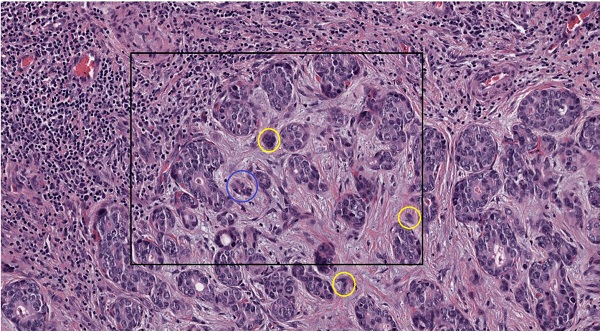
Background: Intrahepatic cholangiocarcinoma (ICC) represents an aggressive carcinoma with a dismal prognosis. For resection specimens, histopathological prognosticators are limited to standard AJCC parameters. Tumor budding (TB), a quantitative leviable parameter for tumor cell separation and infiltration is a promising prognostic factor for several cancers. This retrospective study investigated the prognostic impact of tumor budding in ICC, using a semi-automated approach.
Method: From the Memorial Sloan-Kettering Cancer Center pathology archives, tissue specimens from ICC patients were HE stained and digitized. Tumor budding was analyzed according to the International Tumor Budding Consensus Conference 2016 via QuPath in ten 0.785 mm² vision fields within the tumor center and the tumor-host interface. Within each field, automated QuPath cell detection was conducted and manually reviewed. Tumor budding was correlated with clinico-pathological parameters including AJCC 8th edition classification, hepatitis status, age, ethnicity, treatment, sex, patient overall (OS) and recurrence free survival (RFS) via uni- and multivariate analyses.
Results: From 89 patients, 1780 Vision fields comprising 6006 tumor buds were analyzed and correlated with patients' OS and RFS. The median value for tumor budding in tumor budding hot spots was five within the tumor-host interface and six within the tumor center. Tumor budding correlated significantly with patient OS and RFS in uni- and multivariate analyses (p<0.001).
Conclusion: Our data supports tumor budding, assessed using a digitally enhanced technique, as an independent prognosticator in ICCs for patient's OS and RFS.
Keywords: Intrahepatic cholangiocarcinoma, tumor buds, automated cell detection, independent prognosticator of survival

 Global reach, higher impact
Global reach, higher impact