3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2022; 13(9):2872-2883. doi:10.7150/jca.72021 This issue Cite
Research Paper
LKB1 inhibits proliferation, metastasis and angiogenesis of thyroid cancer by upregulating SIK1
1. Department of Otorhinolaryngology-Head&Neck Surgery, The First Affiliated Hospital of Xi'an Jiaotong University, Xi'an, Shaanxi 710061, China.
2. Department of Clinical Medicine, Medical School of Xian Jiaotong University, Xi'an, Shaanxi 710061, China.
3. Department of Otorhinolaryngology-Head&Neck Surgery, The Second Affiliated Hospital of Xi'an Medical University, Xi'an, Shaanxi, 710038, China.
4. Department of Cardiology, Xianyang Hospital of Yan'an University, Xianyang, Shaanxi Province, 712000, China.
5. Department of Otorhinolaryngology-Head&Neck Surgery, The First Affiliated Hospital of Xi'an Medical University, Xi'an, Shaanxi, 710001, China.
6. Department of Human Anatomy, Histology and Embryology, School of Basic Medical Sciences, Xi'an Jiaotong University Health Science Center, Xi'an, Shaanxi 710061, China.
7. Key Laboratory of Environment and Genes Related to Diseases, Xi'an Jiaotong University, Ministry of Education of China, Xi'an, Shaanxi 710061, China.
8. Department of Vascular Surgery, The First Affiliated Hospital of Xi'an Jiaotong University, Xi'an, Shaanxi 710061, China.
*These two authors contributed equally to this work.
Abstract
Purpose: Liver kinase B1 (LKB1), also known as serine/threonine kinase 11, was considered as a tumor suppressor, which exhibited anti-cancer activity in a variety of cancers. However, the effect of LKB1 in thyroid cancer remains unclear.
Methods: In the study, MTT assay, colony formation assay, flow cytometry, western blot analysis, wound healing assay, transwell assays, quantitative real-time PCR, HUVEC migration assay, ELISA assay, tube formation assay and nude mice xenograft were used to investigate the anti-cancer capacity of LKB1 in thyroid cancer in vitro and in vivo.
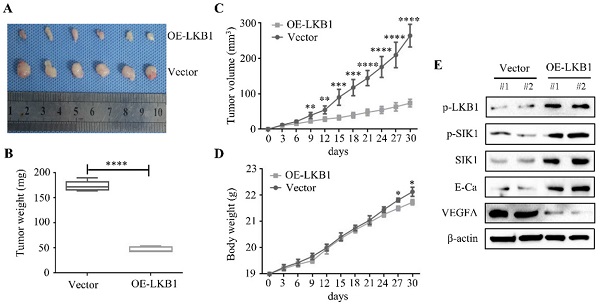
Results: In the present study, we found that the expression of LKB1 was lower in thyroid cancer tissues and cell lines, compared with the adjacent normal tissue and thyroid epithelial cell. After construction of stable clone cells with ectopic LKB1 overexpression, the findings revealed that LKB1 overexpression exerted anti-proliferative and pro-apoptotic property in thyroid cancer TPC-1 and BCPAP cells. In addition, LKB1 overexpression could inhibit migration and invasion, downregulate MMP2 and MMP9 expressions, and reverse EMT in thyroid cancer cells. Furthermore, overexpression of LKB1 attenuated HUVEC recruitment, decreased the expression of VEGFA and inhibited the formation of new vessels in thyroid cancer cells. To validate the underlying mechanism of LKB1 in thyroid cancer, the results showed that LKB1 could positively regulate SIK1 in thyroid cancer TPC-1 and BCPAP cells. Additionally, the SIK1 inhibitor HG-9-91-01 could partially abrogate the anti-proliferative and anti-metastatic effect of LKB1, and reverse MET (mesenchymal-to-epithelial transition) mediated by LKB1 overexpression. Ultimately, the results in vivo revealed that LKB1 overexpression exhibited a strong inhibitory effect of tumorigenicity and presented anti-angiogenic characteristic in nude mice xenograft model.
Conclusion: the results demonstrated that LKB1 could inhibit proliferation, metastasis phenotype and angiogenesis, and reverse EMT in thyroid cancer in vitro and vivo via the upregulation of SIK1, suggesting that LKB1 could be considered as a potential therapeutic target for the treatment of thyroid cancer.
Keywords: LKB1, thyroid cancer, metastasis, EMT, angiogenesis, SIK1

 Global reach, higher impact
Global reach, higher impact