Impact Factor
ISSN: 1837-9664
J Cancer 2022; 13(9):2912-2921. doi:10.7150/jca.50285 This issue Cite
Research Paper
Impact of mismatch repair or microsatellite status on the prognosis and efficacy to chemotherapy in metastatic colorectal cancer patients: A bi-institutional, propensity score-matched study
1. State Key Laboratory of Oncology in South China, Collaborative Innovation Center for Cancer Medicine, Sun Yat-sen University Cancer Center, Guangzhou 510060, P. R. China.
2. Research Unit of Precision Diagnosis and Treatment for Gastrointestinal Cancer, Chinese Academy of Medical Sciences, Guangzhou 510060, P. R. China.
3. Department of Medical Oncology, The Second Affiliated Hospital of Kunming Medical University, 374 Dianmian Avenue Wuhua district, Kunming, 650101, P. R. China.
#These authors contributed equally to this study and share first authorship.
Abstract
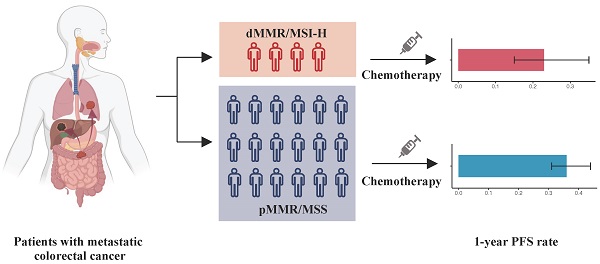
Background: Deficient mismatch repair (dMMR) or the microsatellite instability (MSI) phenotype occupied approximately 15-18% of CRC patients. Previous studies showed that dMMR/MSI status is a favorable prognostic factor for stage II/III CRC patients. For metastatic colorectal cancer (mCRC) patients, only 5% of patients have the dMMR/MSI-H phenotype. The relationship between dMMR/MSI, chemosensitivity and survival in mCRC patients of real-world is still not clear.
Materials and methods: In this study, we enrolled 77 dMMR/MSI-H mCRC patients and compared their clinicopathological characteristics with those of 510 proficient MMR (pMMR) or microsatellite stable (MSS) mCRC patients. With propensity score matching (PSM) analysis, we further compared the chemosensitivity and survival of dMMR/MSI-H mCRC patients with pMMR/MSS patients. We also analyzed the efficacy of different chemotherapy and target therapy in the dMMR/MSI-H population.
Results: In PSM cohort, the objective response rate (ORR) of mCRC patients with dMMR/MSI-H undergoing first-line palliative chemotherapy was 35.2%, which was similar with patients with pMMR/MSS (35.4%, p = 1.00). The median progression-free survival (PFS) of first-line chemotherapy was significantly different (dMMR/MSI-H vs pMMR/MSS = 7.4 months vs 10.2 months; HR = 0.74; 95%CI, 0.57-0.98; p = 0.03). Overall survival (OS) of patients did not significantly differ by status (dMMR/MSI-H vs pMMR/MSS = 40.0 months vs 41.3 months; HR = 1.09; 95%CI, 0.74-1.59; p = 0.68). For second-line palliative chemotherapy, there was no difference in ORR (p = 0.53) or in PFS (HR = 0.88; 95%CI, 0.59-1.33; p = 0.56) between dMMR/MSI-H and pMMR/MSS tumors. We also found that in the overall cohort, the ORR of patients who received oxaliplatin-based and irinotecan-based chemotherapy were 28.8% and 54.5%, respectively, which were not significantly different (p = 0.16). Our results also showed that the use of bevacizumab could lead to a significantly higher ORR in dMMR/MSI-H mCRC patients compared to chemotherapy alone (55.0% vs 22.2%; p = 0.02), whereas cetuximab could not.
Conclusion: The dMMR/MSI-H is not a prognostic factor for mCRC patients but is correlated with shorter PFS to first-line palliative chemotherapy.
Keywords: Colorectal cancer, Deficient mismatch repair, Microsatellite instability, Chemotherapy, Prognosis

 Global reach, higher impact
Global reach, higher impact