Impact Factor
ISSN: 1837-9664
J Cancer 2023; 14(7):1132-1140. doi:10.7150/jca.81675 This issue Cite
Research Paper
Microsatellite Status Detection of Colorectal Cancer: Evaluation of Inconsistency between PCR and IHC
1. Department of Pathology, Xiangya Hospital, Central South University, Changsha, Hunan 410078, China
2. Department of Pathology, School of Basic Medicine, Central South University, Changsha, Hunan 410078, China
3. Cancer Research Institute, School of Basic Medicine, Central South University, Changsha, Hunan, 410078, China
4. Key Laboratory of Carcinogenesis and Cancer Invasion (Central South University), Ministry of Education, Hunan, 410078, China
5. Key Laboratory of Carcinogenesis (Central South University), Ministry of Health, Hunan, 410078, China
Abstract
Objective: An essential component of precision medical treatment for colorectal cancer (CRC) is the use of microsatellite state in combination with polymerase chain reaction (PCR) and immunohistochemistry (IHC) as the primary clinical detection methods. Microsatellite instability-high (MSI-H) or mismatch-repair deficiency (dMMR) accounts for about 15% of all CRC patients. Characterized by a high mutation burden, MSI-H is a predictive biomarker of immune checkpoint inhibitors (ICIs). Misdiagnosis of microsatellite status has been shown to be an important cause of resistance to immune checkpoint inhibitors. Therefore, a rapid and accurate assessment of microsatellite status can be beneficial for precision medicine in CRC.
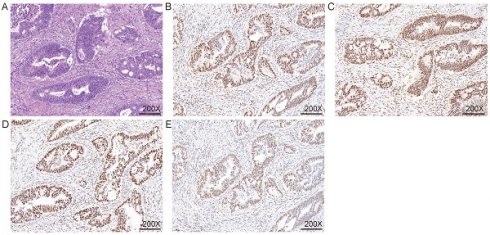
Methods: We evaluated the rate of discordance between PCR and IHC detection of microsatellite status from a cohort of patients that had 855 colorectal cancers. PCR-based microsatellite assay was performed using a set of five monomorphic mononucleotide makers (NR-24, BAT-25, CAT-25, BAT-26, MONO-27) and two polymorphic pentanucleotide (Penta D and Penta E). IHC was used to detect the absence of mismatch repair proteins (MLH1, MSH2, MSH6, and PMS2). The inconsistency rates of the two assays were evaluated.
Results: Among 855 patients,15.6% (134 to 855) cases were identified as MSI-H by PCR, whereas 16.9% (145 to 855) cases were identified as dMMR by IHC. There were 45 patients with discordant results between IHC and PCR. Of these, 17 patients were classified as MSI-H/pMMR and 28 patients as MSS/dMMR. When the clinicopathological characteristics of these 45 patients were compared to those of the 855 patients, it was found that more patients were younger than 65 years old (80% to 63%), more were male (73% to 62%), more were located in the right colon (49% to 32%), and more were poorly differentiated (20% to 15%).
Conclusion: Our study demonstrated a high concordance between the PCR and IHC results. In order to reduce the ineffective treatment of ICIs due to MSI misdiagnosis, the patient's age, gender, tumor location and degree of differentiation should be included in the clinician's selection of MSI testing in colorectal cancer.
Keywords: colorectal cancer, mismatch repair, microsatellite instability, polymerase chain reaction, immunohistochemistry

 Global reach, higher impact
Global reach, higher impact