3.2
Impact Factor
ISSN: 1837-9664
J Cancer 2023; 14(17):3227-3237. doi:10.7150/jca.88009 This issue Cite
Research Paper
Distant Metastasis is the Dominant Cause of Treatment Failure after Lateral Lymph Node Dissection in Patients with Lateral Lymph Node Metastasis: Results of the Large Multicenter Lateral Node Study in China
1. Department of Surgery, Anyang Tumor Hospital, The Affiliated Anyang Tumor Hospital of Henan University of Science and Technology, Anyang, 455000, China.
2. Department of Minimally Invasive Surgery, Beijing Chest Hospital, Capital Medical University, Beijing Tuberculosis and Thoracic Tumor Research Institute, Beijing, 101125, China.
3. Department of Colorectal Surgery, National Cancer Center/National Clinical Research Center for Cancer/Cancer Hospital, Chinese Academy of Medical Sciences and Peking Union Medical College, Beijing, 100021, China.
4. Department of General Surgery, Jilin City Central Hospital, Jilin, Jilin 132001, China
5. Department of General Surgery, Hebei Province Hospital of Chinese Medicine, Affiliated Hospital of Hebei University of Chinese Medicine, Shijiazhuang, 050013, China.
*These authors contributed equally to this work.
Abstract
Background: Lateral lymph node (LLN) metastases (LLNM) are often associated with poor prognosis. This study aimed to investigate the prognostic significance and postoperative recurrence pattern in rectal cancer patients with LLNM after LLN dissection (LLND).
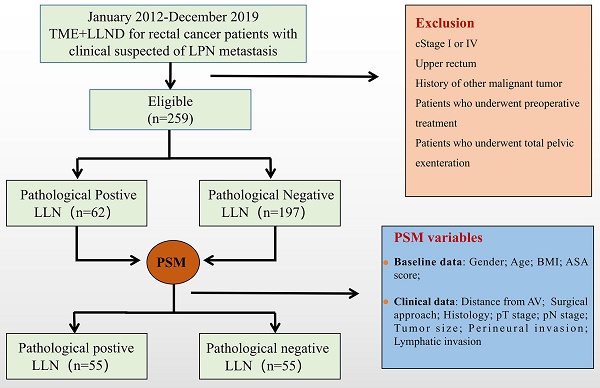
Materials and Methods: This is a multicenter retrospective case-control study where propensity score-matched (PSM) analysis was introduced. From January 2012 to December 2019, 259 patients with clinical suspicion of LLNM who underwent LLND without neoadjuvant therapy were included in the study. They were divided into the negative (n = 197) and positive (n = 62) LLN groups. Primary endpoints were 3-year recurrence-free survival (RFS), local recurrence-free survival (LRFS), and distant metastasis-free survival (DMFS).
Results: After PSM, the DMFS rate in the positive LLN group was significantly worse (67.9 vs. 52.5%, P = 0.012). Pathological LLNM (HR, 3.07; 95% CI, 1.55-6.05; P = 0.001) were independent prognostic factors for DMFS. Patients in the positive LLN group had a higher proportion of distant metastases in all recurrence patterns (92.3% vs 82.6%). Among patients with LLN metastasis, metastases to the common iliac and external iliac arteries were the independent prognostic factor for DMFS (HR: 2.85; 95% CI, 1.31-4.67; P = 0.042). No significant different was observed for prognosis between patients with metastases to the obturator or internal iliac vessels and patients with a N2b stage.
Conclusion: Distant metastasis is the main cause of treatment failure after LLND in patients with LLNM. Because of the low completion rate of adjuvant chemotherapy, preoperative chemotherapy or total neoadjuvant therapy may be considered before LLND. In addition, patients with metastasis to external iliac and common iliac vessels have an extremely poor prognosis, and systemic chemotherapy instead of LLND should be recommended.
Keywords: lateral lymph node metastasis, lateral lymph node dissection, distant metastasis, rectal cancer, preoperative chemotherapy, total neoadjuvant therapy.

 Global reach, higher impact
Global reach, higher impact