Impact Factor
ISSN: 1837-9664
J Cancer 2022; 13(3):965-974. doi:10.7150/jca.65366 This issue Cite
Research Paper
Application of radiomics feature captured from MRI for prediction of recurrence for glioma patients
1. Department of Radiation Oncology, Suzhou Dushu Lake Hospital, Dushu Lake Hospital Affiliated to Soochow University, Medical Center of Soochow University, Suzhou, 225200, China
2. Department of Radiation Oncology, Fudan University Shanghai Cancer Center; Department of Oncology, Shanghai Medical College, Fudan University, Shanghai, 200032, China
#These authors contributed equally
Abstract
Purpose: This study aimed to develop and validate a recurrence prediction of glioma patients through a radiomics feature training and validation model.
Patients and methods: In this study, the prediction model was developed in a training cohort that consisted of 88 patients from January 2014 to July 2017 with pathologically confirmed gliomas. Their pre-radiotherapy and recurrence brain magnetic resonance imaging (MRI) images were collected, and the radiomics features were extracted. Clinical factors including age, gender, WHO grade, Isocitrate dehydrogenases (IDH) mutation status and treatment after surgery were collected. The least absolute shrinkage and selection operator (LASSO) regression model was conducted for data dimension reduction, feature selection, and radiomics feature analysis. Internal validation was assessed. An independent validation cohort contained 41 consecutive patients from August 2017 to December 2018. Furthermore, multivariable logistic regression analysis was used to develop the predicting model by combining the radiomics signature and independent clinical factors.
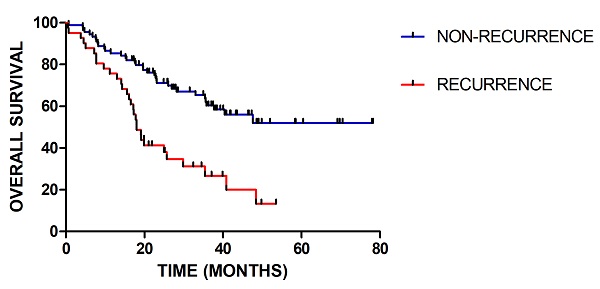
Results: In total, 129 patients were included, among which 40 patients had recurrence. The median follow-up time was 27.4 (range, 2.6-79.2) months. We compared the tumor regions radiomics difference between the recurrence and non-recurrence patients. The radiomics signature was associated with the event of recurrence (P < 0.001 for both training and validation cohorts, respectively). The training model showed good discrimination with a C-index of 0.7578 (95%CI: 0.6549-9.8608) through internal validation on T1 contrast-enhanced magnetic resonance imaging, and a consistent trend in calibration. In the validation cohort, the model also showed good discrimination (C-index, 0.6925, 95%CI: 0.5145-0.8705) and good calibration. In the other two sequences of MRI (T1WI, T2WI), the validation model also showed positive results. Meanwhile, radiomics feature and clinical factors were significantly prognostic for recurrence (P value <0.05, respectively).
Conclusion: We identified the radiomics feature derived from brain MRI that presented potential in predicting recurrence in glioma patients. This could be beneficial to risk stratification for patients. Further investigation is necessary to include expanded sample size investigation and external multicenter validation.
Keywords: gliomas, MRI-based radiomics, recurrence

 Global reach, higher impact
Global reach, higher impact